Impact Factor : 0.548
- NLM ID: 101723284
- OCoLC: 999826537
- LCCN: 2017202541
*Md Sehal Khan Abid and Dr Pravin popatrav bande
Received: October 21, 2017;; Published: October 27, 2017
Corresponding author: Md Sehal Khan Abid, MBBS (AMU) Dip in Orthopedics (AMU), DNB Orthopedics, Bhabha Atomic Research Hospital, Mumbai 94, India
DOI: 10.26717/BJSTR.2017.01.000472
Trigger finger is a common condition with a reported prevalence of 2% to 20% [1,2]. Generally, trigger finger affects women more than men and the age distribution is bimodal with one group below six years of age and the other in their fifth and sixth decade of lif. It is a disorder which is associated with entrapment of the flexor digitorum superficialis or flexor digitorum profundus tendon along its course through fibro-osseous tunnels of the wrist, palm and digits of the hand [1]. Onset is usually gradual, associated with repetitive tasks, unaccustomed activity or compression of the pulley against hard objects. Snapping, clicking, locking, stiffness, and difficulty extending a flexed digit, often with discomfort or pain, are the most prominent symptoms [3,4]. Several studies suggest that individuals with type 1 diabetes, rheumatoid arthritis, carpal tunnel syndrome, arthritic changes in the wrist, hypothyroidism, mucopolysaccharidoses, amyloidosis, and congestive heart failure may be predisposed to flexor tendon entrapment [1].
The research on patients with trigger finger indicates various methods of treating patients including splinting, nonsteroidal antiinflammatory agents, percutaneous injection of corticosteroids, and surgical releas [1,2,5]. Very small, uncontrolled case series have shown in their results that only about half of patients are satisfied with their symptoms after a period of splint immobilization [6-8]. Triggering may resolve after one or two corticosteroid injections, but the results vary substantially between studies (35 % and 87 % for one and 72 % to 92 % for two injections) [9-13]. Various literatures suggest that patients should be informed about 50% success rates when offering a corticosteroid injection for trigger finger and that the chances of patients landing to surgical release still remains [14-16]. Percutaneous release has a success rate of 94% according to a recent systematic review of 2114 procedures but is accompanied by relatively high rates of complications like injury to nerves, injury to A2 pulley and bowstringing [17]. Open surgical release has a high success rate with few adverse events and is supposed to be the final treatment for trigger fingers [18,19]. We here present a case of trigger finger which has unique presentation but is successfully treated with open release.
Figure 1: Release of A1 pulley of right thumb.
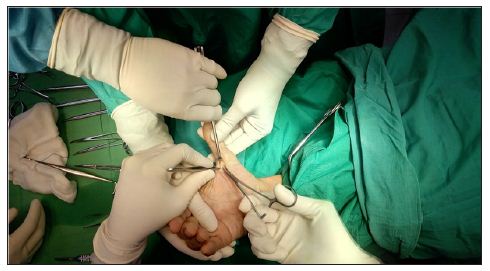
Figure 2: Release of A1 pulley of right thumb.
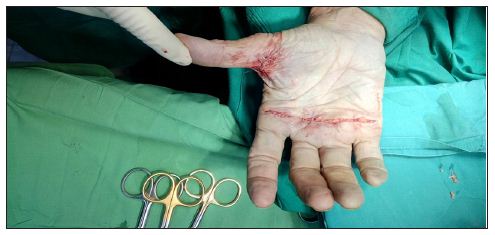
An 80 years old male patient presented to our OPD with triggering of both thumbs and middle finger of left hand. The patient had no co morbidities like diabetes, hypertension, or hypothyroidism and hence was advised percutaneous steroid injections along with analgesics and relative splinting. 2 weeks after the injection he was relieved of his symptoms in left thumb and middle finger but right thumb was still affected. The patient was advised 2nd dose of subcutaneous steroid injection along the flexor tendon sheath and A1 pulley of right thumb but his symptoms still persisted. As the patient was still reluctant to undergo surgical release he was offered splinting and relative rest to the thumb. After 2 months of initial presentation he again present to our OPD with triggering and pain at A1 pulleys of all fingers in right hand and remaining 3 fingers in the left hand. He was finally operated with release of A1 pulley of all fingers in right hand and steroid injections in left hand. After 3 months of surgery the patient was doing well with good finger grip and no pain or restriction of movements. The operative pictures and surgical approach has been shown in (Figures 1 & 2).
The present case is unique in itself with only one case reported till date as triggering of 10 fingers [20]. Although the presentation was gradual and the treatment was staged with physiotherapy, steroid injection and finally with surgical open release but eventually all the fingers were involved in a period of 3 months and they needed some form of intervention. Two out of three fingers which were initially treated by steroid injections were cured with no symptoms after 3 months of presentation. This result is similar to the published data about the efficacy of steroid injections in treatment of trigger fingers [9-11]. Patients who have recurrence or treatment failure with steroid injections are usually seen to opt for surgery in the first place, if other fingers are involved. Similar is the situation in our case where the patient opted for surgical release when remaining fingers were involved.
Trezies et al. investigated the occupational histories of 178 patients with idiopathic trigger fingers and they demonstrated no significant difference between the occupational distribution of patients with trigger digits and that of the general population [21]. They concluded that occupation may have a role to play in triggering of digits but many patients develop trigger for reasons other than occupation. Weilby concluded that anatomic and intrinsic factors, contribute to a predisposition for the development of tendon entrapment of the hand [22]. Our patient was a male who did not have any predisposing factors such as thyroid disease, diabetes, renal disease, connective tissue disorders, gout or rheumatoid arthritis. The unusual presentation of this patient at the age of 80 years with no positive family history and with no occupational predisposition for trigger finger makes this case unique in itself.
Trigger finger is a condition characterized by fibrocartilagenous metaplasia and hypertrophy of the surrounding structures of the flexor tendon resulting in a painful and debilitating restriction of motion. Flexor tendinopathy could be multi-factorial including anatomical variations of the pulley system and biomechanical etiologies. This could be exposure to shear forces and unaccustomed activity. Conventional treatment aims at decreasing inflammation through corticosteroid injection or surgically removing imposing tissue. Steroids although serve as a non surgical means to relieve the patient of symptoms, but have a limited role in multiple trigger digits presenting at one setting.


