Impact Factor : 0.548
- NLM ID: 101723284
- OCoLC: 999826537
- LCCN: 2017202541
Anshuman K Gupta and Vasudeva S Pai*
Received: January 06, 2018; Published: January 16, 2018
*Corresponding author: Vasudeva S Pai, PO Box: 97395 Ronwood Av, Manukau Auckland 2241, New Zealand
DOI: 10.26717/BJSTR.2018.02.000659
Abbreviations: CRPS : Complex Regional Pain Syndrome; FBSS: Failed Back Surgery Syndrome; SCS : Spinal Cord Stimulator; IASP: International Association for the Study of Pain
Complex regional pain syndrome (CRPS) is a known long term pain syndrome known to originate from trauma, nerve injury or post operation. Subtypes include type 1 (develops following a noxious stimuli which may or may not be trauma related) and type 2 (develops after nerve injury). Type 1 CRPS has been well described after hand or foot surgeries and sometimes after a total knee joint replacement. In this condition there is intractable pain and avoidance of long term sequelae is best achieved through early diagnosis and active treatment. Despite the evident progress in treating lumbar degenerative diseases, the rate of a so-called “Failed back surgery syndrome” [FBSS] remains relatively high and varies from 10% to 40% [1]. Type 2 Complex regional pain syndrome (CRPS II) in the presence of failed back syndrome following a lumbar surgery is confusing and is not easy to diagnose.
Istrelov concluded that in the majority of cases, the cause of the residual or recurrent pain could be identified. They suggested that causes of failed back syndrome were related to unrecognized lateral recess stenosis, facet arthritis or myofascial pain, recurrent disc herniation or epidural scaring as the causation of the syndrome [1]. We report 3 diagnosed cases of CRPS Type II, which developed after discectomy/fusion surgery of lumbar spine, suggesting although uncommon, is not rare. The difficulty in recognition and its treatment had been emphasized with a high clinical index of suspicion and careful assessment being required for early diagnosis. The CRPS was diagnosed with the exclusion of the causes of postoperative syndrome or a failed back syndrome in the lumbar spine such as recurrent disc herniation, epidural fibrosis, persistent spinal stenosis or spinal instability. The need for multidisciplinary pain management was emphasized.
A 48-year old normally fit woman presents with 2 weeks of progressive back pain and stiffness. In the week leading up to this she describes having felt a back pain after lifting a lawn mower to put it on a trailer but thought nothing of it. The progressive nature of the pain caused her to present to the Emergency department where she had an MRI performed of her lumbar spine that showed extruded disc at L3-L4 level. She had two CT guided steroid injections with no relief of symptoms. Subsequent assessments by orthopedic surgeons suggested she had developed worsening left anterior thigh and knee pain. Clinical examination revealed marked hypoesthesia over the left L3 dermatome with associated reduced left knee jerk reflex. Knee extension power was difficult to assess because of pain.
Figure 1: MRI Lumbar spine demonstrating reduced L3/4 intervertebral disc space with protrusion and possible adjacent vertebral body abscess.
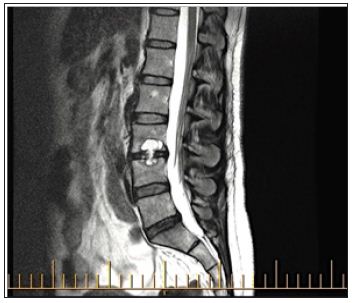
A repeat MRI showed a reduced L3/4 intervertebral disc space with protrusion of the disc suggestive of discitis with an adjacent vertebral body abscess (Figure 1). Blood investigations did reveal normal ESR and CRP with CT guided biopsy at L3/4 not revealing any polymorphs or organisms on culture. No acid fast bacilli were grown on Mycobacterial culture. Her back and left leg pain continued. She underwent open biopsy, bone grafting and fusion of L3-L4 with pedicle system. Intra-operatively there was no evidence of infection with histology showing a ganglion cyst. After surgery, her back pain eased with medication; however her anterior thigh and knee pain increased considerably and was persisting 6 months’ post operatively. A post-operative MRI of the spine and knee was unremarkable with no abnormalities on blood investigations.
A second opinion was sought and on examination she was found to have an antalgic gait, mobilizing with two crutches and only being able to touch weight bear on her left knee. She was also very stiff in the left knee with movement of 30 degrees from fixed flexion of 20 degrees. Palpation, muscle testing and knee reflexes were not possible because of hyperesthesia around the knee. Associated shiny skin colour changes around this area were also noted. These changes fit into a diagnosis of chronic regional pain syndrome. We performed electromyography of the lower extremities and the results showed chronic L3 radiculopathy. The 3-phase bone scan showed only non¬specific findings. On an updated MRI of the lumbar spine, there was no evidence of focal disc herniation and compression of the thecal sac or nerve root, and the fixation device was in good position according to the contrast enhancement lumbar MRI findings.
A diagnosis of neurogenic type 2 CRPS from chronic irritation of L3 nerve root was made. She was referred to the pain team for pain management where she received analgesia in the form of anti- inflammatory drugs and gabapentin with the physiotherapist assessment for TENS, grade desensitization therapy and mobilization with feedback. She was provided psychological consultation and antidepressants at the neuropsychology centre. Furthermore, the patient received local injection therapy that included epidural block at the pain clinic, but she did not show any satisfying improvement of the symptoms. Presently she has been considered for a permanent spinal cord stimulator as she had a successful trial of stimulation with a temporarily (1 week) implanted electrode.
A 51-year-old ex-registered nurse who underwent a microdiscectomy for disc herniation at L5/S1 for an irritating nerve root causing sciatic pain down her right side. She showed good post-operative improvement initially which allowed her to return to work within a week. Approximately three months later she suffered an episode of trauma to the right side which caused a return of paraesthesia in the right foot with associated sharp intense pain in the right leg. An MRI revealed epidural scarring but no recurrent disc herniation. She was treated by the pain team and referred for a second opinion. At the time of her second opinion, she had a severe form of CRPS with a completely non- functional right leg. She was mobilising non-weight bearing on two crutches.
Multiple non- healing ulcers with a swollen shiny equinus right foot with a very sensitive leg from the proximal third of the leg was noted on examination. She still had a good functioning knee, but could not fully straighten it because of pain radiating to her right leg. Her impairment was primarily due to regional pain syndrome of her right leg. She was wheel chair bound at the time of assessment. Clinically she was consistent with CRPS type II with involvement of right L5 nerve root irritation. She failed to respond to various modalities of treatment by the multidisciplinary pain clinic. As there was no easy solution for her on going severe pain, she was given two options -1. To continue pain medication and mobilize with a wheelchair. 2.To consider amputation with an understanding that the amputating would not completely cure her CRPS pain but would at least prevent the harmful effects of the vascular ulcers and further deterioration of pain. She opted for the second option.
A 56 year old female with a past history of 4 surgeries for her left-sided sciatica in the late 1990’s which had left her with a residual left foot drop, presented with knee and ankle pain following fall at work. A partial tear of the patellar tendon was suspected but this had been ruled out on MRI. Her left knee pain improved, however her left foot symptoms persisted. A diagnosis of Morton’s neuronal was made and was treated with local cortisone injection without any improvement as her left foot pain worsened
on second opinion, it was noted that she had clicks and clunks in both knees, but had reasonable and symmetrical movements bilaterally with no reported or observed pain. Clinical examination of her foot showed there were definite colour changes from the knee down with associated diffuse swelling of the foot and bruising between the third and fourth toe ray near the web space.
Her skin was not shiny and there was no excessive sweating, but her left leg felt colder when compared to the right. Her partner stated that he noticed these changes after her cortisone injection in the third intermetatarsal space. In addition, her pain was more generalized and intense than that could be explained based on her stated injury or Morton’s neuronal. In our opinion, it was more than likely there was an early onset of CRPS type 2 related to left L5 nerve root [which was initially damaged following surgery of 1990’]. Her twisting injury or digital nerve irritation from injection likely precipitated her symptoms. She was referred to a pain-team for further management.
`The increasing number of spinal surgeries through the years has seen a corresponding increasing trend in the cases of failed back surgery syndrome [FBSS] in the lumbar spine. FBSS is now reported to have a 15% chance of occurring following surgeries for the back [2,3]. The causes of FBSS have been well reported. These are related to selection of incorrect patients for lumbar procedures, incorrect clinical diagnosis, the technical problems and the wrong procedure during the operation, postoperative infection, recurrent disc herniation, spinal instability, scar adhesion, adhesive arachnoiditis, and failure of fusion and problems of the fixation device. We described three cases CRPS Type II following lumbar spinal surgery, which previously have been rarely reported [4]. Despite spinal surgery, the symptoms did not improve and were grouped under FBSS. A second opinion in all three above cases revealed CRPS II, thus indicating complexity in diagnosis.
CRPS is a neurogenic pain that is caused by trauma, fracture, operation, nerve injury etc. It is characterized by various types of pain, functional loss, edema and dystrophic changes [5,6]. There is no single proven diagnostic tool, but taking a detailed history and understanding the chief complaint along with the use of simple radiography, 3-phase bone scanning and infrared thermography can help to diagnose CRPS. However, the most important thing is the clinical decision with the exclusion of other diagnosis. The International Association for the Study of Pain (IASP) named and divided CRPS into type 1 and type 2. Type 1 is without nerve injury after soft tissue injury, and type 2 is related to the nerve injury.
The Budapest group for CRPS suggested that the following criteria must be met for the diagnosis:
a) Continuing pain, which is disproportionate to any inciting event
b) Must report at least one symptom in three of the four following categories:
i. Sensory: Reports of hyperesthesia and/or allodynia
ii. Vasomotor: Reports of temperature asymmetry and/or skin color changes
iii. Sudomotor/Edema: Reports of edema and/or sweating changes
iv. Motor: Reports of decreased range of motion and/or motor dysfunction (weakness, tremor, dystonia) and/or trophic changes (hair, nail, skin)
c) Must display at least one sign at time of evaluation in two or more of the following categories:
i. Sensory: Evidence of hyperalgesia (to pinprick) and/or allodynia
ii. Vasomotor: Evidence of temperature asymmetry (>1°C)
iii. Sudomotor/Edema: Evidence of edema and/or sweating changes and/or sweating asymmetry
iv. Motor/Trophic: Evidence of decreased range of motion and/or motor dysfunction (weakness, tremor, dystonia) and/or trophic changes (hair, nail, skin)
d) There is no other diagnosis that better explains the signs and symptoms
The principles of CRPS treatment lie in an early diagnosis, physical therapy and psychological consultation to stabilize the patient’s mental state. There are also adjuvant medicinal treatments [gabapentin, amitriptyline], sympathetic nerve block, epidural block, TENS machine and Spinal cord stimulator [SCS]. In case 1, the patient did not improve with conservative medicinal treatments and various nerve blocks, so we recommended SCS [7,8]. After her fusion surgery she developed CRPS type 2 of the left knee related to an L3 nerve root irritation likely secondary to an L3/4 disc extrusion noticed on MRI in 2012 and 2013. Similarly, in case 2 and 3 symptoms developed in the radicular area of the initial nerve root damage. In addition to early diagnosis for treatment purposes, it is also important to provide these patients with an early multidisciplinary approach such as referring them to a pain clinic.
In our opinion differentiating post-operative syndrome in the lumbar spine from CRPS is difficult and is under diagnosed. We recommend a high clinical index of suspicion for CRPS as the cause of any ongoing post-operative syndrome with neurology after intervention. In the three cases presented, CRPS type II was diagnosed after discovery of ongoing regional symptoms with associated radicular nerve distribution. This report highlights several important points related to the evaluation and management of these difficult problems. Firstly, the diagnosis of CRPS must include a detailed history and careful neurologic examination. It is important to use the accepted diagnostic criteria. When diagnostic criteria are equivocal, other characteristic changes on plain radiography, triple phase bone scintigraphy, thermography or sudomotor and vasomotor studies should be considered.


