Impact Factor : 0.548
- NLM ID: 101723284
- OCoLC: 999826537
- LCCN: 2017202541
Eduardo de Oliveira Duque-Estrada MD*
Received: January 17, 2018; Published: January 25, 2018
*Corresponding author: Eduardo de Oliveira Duque-Estrada, Ex-Professor of Pediatrics and Pediatric Surgery, Teresópolis Schoolof Medicine, Rio de Janeiro, Rua Jose da Silva Ribeiro 119 apt 11 São Paulo, SP Brazil CEP: 05726-130
DOI: 10.26717/BJSTR.2018.02.000695
The local anesthetics are widely u sed in minor pediatric surgical procedures. The major problem with their use is the resulted pain experienced by the patients at the time of injection. To discuss those situations in the light of the medical literature we present this mini-review.
Keywords: Local Injection; Pain; Buffer; pH; Lidocaine; Pediatric Surgery Procedure
Local anesthetics are widely utilized in the practice of pediatric surgical procedures for achieving cutaneous anesthesia both without and with minimal side effects. However, pain or burning sensation at the time of injection is one of the major adverse issues related [1]. The use of 1% lidocaine as a diluent reduces the amount of pain by approximately 75%, although some people still experience substantial pain [2]. The objective of minimizing the pediatric patient discomfort during the application of anesthetic solutions has been considered fundamental in the accomplishment and success of surgical procedures under local anesthesia [3]. A variety of techniques have been used to reduce the pain of infiltration of local anesthetic agents [4,5] including anesthetic solution– related techniques such as buffering the solution with sodium bicarbonate [6-11] fresh mixing of lidocaine with epinephrine [12,13] and warming the solution [14]. Alternative techniques such as distraction [15], altering the rate of infiltration, [16] and a eutectic mixture of lidocaine and prilocaine (EMLA) cream [17] before infiltration, and local external cooling (cryoanalgesia) have also been used to reduce the pain of infiltration of local anesthetic solution [18,19] (Table 1).
Table 1: Techniques for injection pain control*.
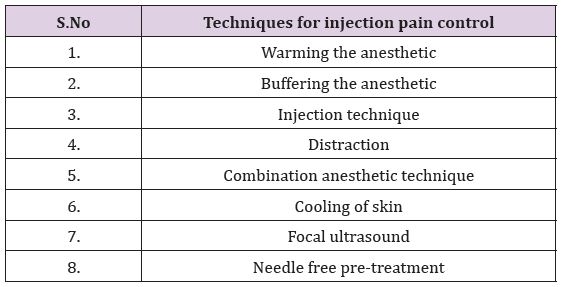
Note: *adapted from Salati SA [1].
Local anesthesia is extremely useful either as the sole method the best results on the minor surgery in general [3,6]. Blocking the pain pathway with local anesthetic solution will also reduce the “family stress response” to the surgical procedure. During our last 30 years of medical practice, and mainly of local pediatric surgery procedures like small procedures, such as suturing of lacerations, removal of cutaneous lesions, and a broad spectrum of office-based procedures we have adopted most frequently the use of local anesthetic practice with lidocaine (1% or 2%) without epinephrine 1: 100,000.We adopted the Buffering lidocaineis more rapidly acting without, having effect in 2 to 3 min, considering the maximum dose is 3 mg/kg. The pH of this product (pH4.2) is, however, approximately 1000 times more acidic than subcutaneous tissue (pH7.4) and this acidity contributes to uncomfortable stinging and burning infiltration [20]. Buffering with sodium bicarbonate (NaHCO3) 8.4%in a 10:1 or 9:1 ratio (10 or 9 parts lidocaine1% containing 5 microgram/ml to 1 part sodium bicarbonate containing 8.4g/l) more closely matches the neutral pH (around 7.4) decreases injection pain.
Basic pH solutions convert lidocaine into its active, alkalinizing the anesthetic mixture also decreases the time of onset of its effects [21]. Commercially available lidocaine comes as an acidic solutionto enhance its stability, but the low pH reduces the amount ofactive drug, and Buffering lidocaine with sodium bicarbonate increasesthe pH to approximately 7.4 [22]. Such an increase inpH in turn increases the amount of pharmacologically activelidocaine, resulting in more effective anesthesia [23]. However, Ong et al. suggested that increasing pH in buffered lidocaineis unable to fully explain the minimization of pain on injection [24]. By the other side, the buffering anesthesic decreases the usual shelf life. Momsen et al. [25] established that the buffered lignocaine epinephrine was stable for up to 24 hours after preparation [25]. Hence, some studies have recommended the preparation of a freshly buffered mixture prior to injection [26]. The antibacterial activity of lidocaine has however, not been found to get diminished by the bicarbonate buffer [27].
As a result, the overall experience perceived by our small patients, adolescents, and the mentally and physically disabled undergoing surgical procedures is improved when local anesthesia is painless or even very reduced. The main medical principle to do no harm, primum non nocere always new.


