Impact Factor : 0.548
- NLM ID: 101723284
- OCoLC: 999826537
- LCCN: 2017202541
Gyanendra Kumar Jha*
Received: February 27, 2018; Published: March 12, 2018
*Corresponding author: Gyanendra Kumar Jha, Lecturer Department of Orthopaedics, College of Medical Sciences, Bharatpur Chitwan, Nepal, India
DOI: 10.26717/BJSTR.2018.03.000848
Introduction: Fractures of distal femur are one of the most prevalent fractures encountered in high-velocity trauma which are associated with high morbidity and mortality if not managed well. The isolated fracture can itself lead to complications such as Acute Respiratory Distress Syndrome (ARDS) and pulmonary embolism (PE). This necessitates early stabilization of fractures. Open reduction and internal fixation (ORIF) with locking compression plate is the treatment of choice for closed fractures of the distal femur. Distal femur anatomic contoured locking compression plate (LCP) has shown to give one of the best results regarding recovery, fracture union, return to work and the functional outcome. We present our experience of management of distal femur fracture at our centre.
Methods: 30 cases of supracondylar femur fracture were treated by ORIF with LCP between 1st October 2014 to 30th September 2016 at our tertiary level trauma centre. The patients were evaluated clinically and radiologically for outcomes. All patients were followed up for an average of 6 months. The outcome was assessed using Neer's Score. The fracture was considered united clinically when there was no pain on palpation, no discomfort on full weight bearing. Radiologically fracture was considered united when serial roentgenograms demonstrated bone trabaculae is crossing the fracture site. The functional outcome was evaluated by Neer's knee score criteria.
Result: In our study 30 cases of supracondylar femur fractures were treated. 18 patients were males, and 12 patients were females. The median age was 34.97 years ranging from 18 to 62 years? All the fractures were caused by road traffic accidents. 19 patients were with fracture on the right side and 11 on the left side. Using Neer's scoring system excellent outcome was seen in 53.33%, good in 36.67%, fair in 6.67% and failure in 3.33%. The range of motion of the knee was excellent to very good. Gait and weight bearing after the complete union was satisfactory.
Conclusion: The method of treatment is standard with good exposure of fracture fragments, less operative time and good functional and radiological outcome. LCP is an important modality in the treatment of fractures around knee especially when the fracture is severely communited and in situations of osteoporosis.
Keywords: Supracondylar fracture; locking compression plate; Open reduction internal fixation
Abbreviations: ARDS: Acute Respiratory Distress Syndrome; PE: Pulmonary Embolism; ORIF: Open Reduction and Internal fixation; LCP: Locking Compression Plate
Distal femoral fractures currently account for less than 1% of all fractures and about 3% to 6% of all femoral fractures; however, the incidence rate increases with increasing age [1-3]. The distal femur fractures have bimodal incidence. One group includes patients below 40 years of age (nearly 40 % of cases), predominantly males, sustaining high-energy trauma such as Road traffic accident or a fall from heights and the other group consists of patients more than 50 years, (nearly 60 % of cases) predominantly females, with osteoporosis, who sustain relatively low energy trauma [4-8]. However, in both instances, axial load to the leg is the most common cause. Management of distal femoral fracture remains a challenge to orthopaedic surgeons. They usually result from high-velocity injury leading to comminuted and unstable fracture pattern [9,10]. Challenges associated with these types of fractures are adequate exposure of particular surface, particularly of the medial femoral condoyle and coronal plane fractures. In the setting of medial combinations and short distal segment, there is a high incidence of loss of fixation and varus collapse on weight bearing if improper and inadequate fixation technique is used for the treatment of such fractures.
Similarly, these fractures are also associated with higher incidence of infections, joint stiffness, melanin and early onset of osteoarthritis. So these fractures have to be appropriately managed to overcome these factors [11-15]. This led to the concept of indirect reduction and biological fixation of fractures with preservation of vascularises and soft tissue integrity to the bone fragments [1621]. Principle's of management includes anatomic restoration, axial alignment and rotational stability of particular surface. The management of distal femur fracture with anatomical distal locking compression plate (LCP) has multiple benefits. It provides multiple points of fixed plate to screw contact, generating greater stability than is provided by a single lateral construct, which potentially reduces the tendency for varus collapse. The locking screws also provide stronger fixation of the plate in the proximal fragment by eliminating any potential for toggle and sequential screw loosening. These have a particular advantage in osteoporotic bone and have a possible biological advantage over conventional plates [22]. There was no local study available to assess the results of LCP for the management of this types of fractures in our part of the world having the different demographic combination. This study was carried out to assess the functional and radiological outcome of patients with supracondylar femur fracture managed with LCP.
Figure 1: Pre op X-ray Anteroposterior(AP) and lateral X�Ray of thigh.
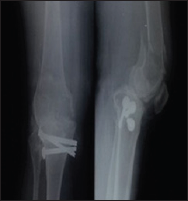
30 cases of supracondylar femur fracture were treated by open reduction and internal fixation (ORIF) with LCP between 1st October 2014 to 30th September 2016 at our tertiary level trauma centre. The patients were evaluated clinically and radiologically for outcomes using various parameters. The fracture was classified according to the AO classification system preoperatively on the Anteroposterior and lateral X-Rays (Figure 1). All the patients in this study were treated by open reduction and internal fixation by using standard lateral approach within four days of injury (Figure 2). The fracture was adequately exposed and reduced under C-arm guidance. K-wires were used to provisionally fix the fracture (Figures 3 & 4). LCP of appropriate length was used in each case according to the type of fracture (Figure 5). All patients were followed up for an average of 6 months. Check X-Ray was done at regular intervals to see the progress of the fracture union (Figures 6-8). The outcome was assessed using Neer's Score [23-26]. The fracture was considered united clinically when there was no pain on palpation, no discomfort on full weight bearing. Radiologically fracture was considered united when serial roentgenograms demonstrated bone trabaculae is crossing the fracture site. The functional outcome was evaluated by Neer's knee score criteria.
Figure 2: Incission.
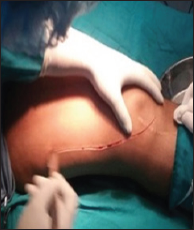
Figure 3: Fracture reduction.

Figure 4: Intraoperative C arm picture.
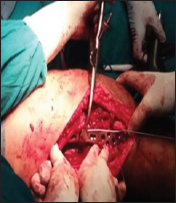
Figure 5: LCP with screws placed over fracture.
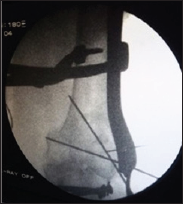
Figure 6: Followup Anteroposterior(AP) and lateral X�Ray of thigh at 24 weeks.
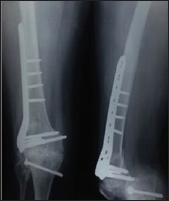
Figure 7: Clinical image showing extension at 24 weeks.
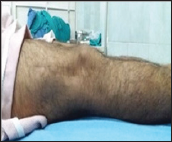
Figure 8: Cinical image showing flexion at 24 weeks.
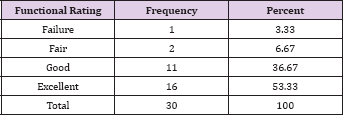
The mean age of 30 treated patients was 34.97 years (range 18-62 years), 18 were male, and 12 were female, 19 patients had a fracture in the right side and 11 on the left side. The number of patients in each fracture type is described in Table 1. All the 30 fractures were closed type fractures. Average blood loss was 85.33 ml (range 50-150ml). The average duration of surgery was 93.83 minutes (range 60-150 minutes). Average flexion achieved by the patients in this study is 103.5° (range 60- 120°). The average duration of full weight bearing was 16.3 weeks (range 14-20 weeks). Average duration of radiological union was 17.83 weeks (range 16-22 weeks) as described in Table 2. 20 percent cases had varus misalignment out of which only 6.7 percent had more than 5 degree of varus misalignment as described in Table 3. 16.7 percent of cases had values misalignment out of which 6.6 percent had more than 5 degree of values misalignment (Table 4). 10 percent cases had knee extension lag out of which only 6.25 percent cases had more than 5 degrees of extension lag. Average Neer score was 83.467 (range 47- 96). Out of 30 cases of supracondylar fracture 16 patients had an excellent outcome, 11 patients had good outcome, two had fair and one case had failure outcome. Out of the 17 cases of AO type, a fracture 14 had excellent outcome and three cases had a good outcome. Out of the 13 cases of AO type three fractures two had excellent outcome eight had good outcome, two had fair outcome and only one had failure outcome (Table 5).
Table 1: Type of Fracture.
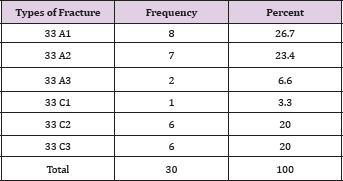
Table 2: Radiological Union.
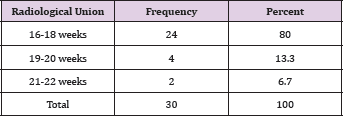

Table 3: Varus Malalignment.
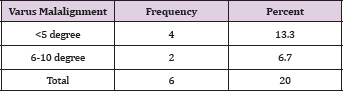
Table 4: Valgus Malalignment.
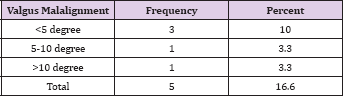

Table 5: Functional Rating.

Intraarticular fractures require anatomic restoration and maintenance of the congruence of the two particular surfaces. Distal femoral alignment is one of the treatment priorities. The femoral shaft is oriented 7° of values in relation to the knee joint. Maintaining this alignment is critical to the function and durability of the limb [27-29]. Coronal plane alignment has been shown to be the most difficult factor to control and the most crucial to the overall outcome [30-32]. Malalignment in the axial and sagittal planes also affects knee kinematics and range of motion. When combination is present, supracondylar femoral fractures are especially prone to varus collapse [33,34] Patients with more significant loss of fixation tend to have a worse outcome. Open fractures are related to high- energy injury mechanism and a higher prevalence of infection. The outcome of distal femoral fractures, similar to other major injuries, not only depends on bony reconstruction but also on soft tissue management. The locking compression plate offers some advantages in fracture fixation combining angular stability through the use of locking screws with conventional plating and bridging plate osteosynthesis [35].
However, the system is complex, requiring careful attention to biomechanical principles and good surgical technique. The angular stability provided by LCP at the plate-screw interface, allows extraperiosteal fixation of the plate to bone. By preserving periosteum blood supply to the bone, it addresses the importance of the biological factors involved in fracture healing. The principles of flexible fixation are employed where the goal is for indirect healing with the formation of callus. Although the LCP system offers a number of advantages in fracture management, its successful use requires careful pre-operative planning, consideration of biomechanical principles, and the use of the appropriate plate and screws combined with good surgical technique. A study conducted by [36] showed that mean age group for distal femur fracture was 35 years. Similarly, in the studies conducted by [37], it was found to be 44 years [38], 40.22 years [39], 44 years [40], 40.44 years [41], 32.37 years. In our study, the mean age group is 34.97 years which can be attributed to the high incidence of road traffic accident in the younger age group which is very common in this part of the country due to its proximity to the east-west highway [42]. In the study conducted by [43] 64 percent of patients were male. Similarly in the study conducted by [44] 76 percent of patients were male, and in the study conducted of 69.2 percent cases were male.
It is comparable to our study in which 60 percent cases were male, and 40 percent were female. This can be attributed to the fact that all the cases in our study were due to road traffic accident. A study conducted by [45] showed that average surgery injury interval was five days. Similarly, in the study conducted by [46], it was seven days, [47] 9.9 days [48], 7.16 days [49], 6.1 days. They concluded that any delay in surgery injury interval predisposes to unsatisfactory results compared to those cases which were done earlier. This is also comparable to our study in which all the cases were managed with five days of injury. A study conducted by [50] showed that average duration of surgery was 85 min with a range of 40-135 min. In the studies by [51] average time was 119.2 minutes with a range of 80-180 minutes, and [52] 129.6 minutes.
They concluded that longer duration of surgery is associated with higher incidence of complications such as infections, delayed or non-union and impaired functional outcome. It is comparable to our study in which average duration of surgery was 93.83 minutes and range of 60-150 minutes. A study conducted by Panchal et al. [53,54] showed that 70% of patients started full wt bearing at 14 weeks. Similarly, Khurseed et al. [55] found it to be 14.32 weeks. In our study it was found to be 16.3 weeks. This can be attributed to the patient factor. The patients were not compliant and started delayed weight bearing for fear of losing the stability from patient side. A study by Krishna et al. [56] showed that average duration of radiological union was 15.36 weeks [56]. Similarly in the study conducted by Malik A et al. [57] showed that 96 % of patients achieved radiological union by 20 weeks and 100 % achieved union by 24 to 36 weeks of follow up, Panchal et al. [53] showed that 85% patients achieved radiological union by 18 weeks, Weight and Collinge [58] found it to be 13 weeks, Kregor et al. [59] found it to be 12 weeks, Bae et al. [60] found it to be 14.3 weeks, Khurseed et al. [55] found it to be 16.88 weeks, Kiran et al. [61] found it to be 14 weeks, Shriharsha et al. [62] found it to be 18.53 weeks, Yeap and Deepak [63] found it to be 18 weeks, Malik I et al. [64] found it to be 13.88 weeks, Malik A et al. [57] found it to be 16 weeks.
In our study mean duration of radiological union was 17.83 weeks and 93.3% of patients achieved radiological union by 20 weeks and 100% achieved union by 22 weeks. The higher union time compared to some ofthe study can be attributed to the fact that all of the cases in our study were managed by open reduction and not by minimally invasive technique. Normal knee flexion is 140°. Laubenthal [65] has demonstrated that average motion required for normal Sitting is 93°, stair climbing is 100° and squatting is 117°. In the study conducted by Krishna et al. [56] average range of knee flexion obtained postoperatively was 111.30°. Similarly in studies conducted by Siliski et al. [66] it was found to be 107 °, Scutz et al. [67] found it to be 103°, Kregor et al. [68] found it to be 109°, Shriharsha et al. [69] found it to be 99°, Bohra et al. [18] found it to be 111°, Yeap and Deepak [64] found it to be 107.7°, Malik I et al. [65] found it to be 107.6°. In our study average knee flexion achieved was 103.5°. Slightly less average knee flexion in some of the patients can be attributed to the fact that some of the patients had multiple injuries involving both distal femur and proximal tibia and some of the patients were not regular with their physiotherapy and knee range of motion exercises.
A study conducted by Panchal et al. [53] showed that 15% of patients had extensor lag more than 10 degrees and 60% had extensor lag less than 5 degrees [53]. Similarly in the study conducted by Scutz et al. [69] 4 percent patients had extensor lag of more than 5 degrees. In our study 3.75 percent cases had extensor lag of less than 5 degree and 6.25 percent cases had more than 5 degrees of extensor lag. A study conducted by Scutz et al. [69] showed that 20 percent cases had less than 10 degrees of varus misalignment which is comparable to our study in which 6.7 percent of cases had more than 5 degrees of varus misalignment. A study conducted by Scutz et al. [69] showed that 3.2 percent cases had more than10 degrees of values misalignment which is comparable to our study in which 3.3 percent cases had more than 10 degrees of values misalignment. A study conducted by Krishna et al. [56] showed that Mean Neer's score was 80.20. It is comparable to our study in which Mean Neer's score was 83.4.
A study conducted by Krishna et al. [56] showed that excellent results were seen in 15 cases, good in 11, satisfactory in 3 and 1 case of failure was seen. Similarly in the study conducted by Shriharsha et al. [69] 80% type A and 40% Type C fractures had excellent or good results. They concluded that extra articular (type A) fractures had better outcome than intra articular (type C) fractures. In the study conducted by Yeap and Deepak et al. [64] 4 patients showed excellent results, 4 good, 2 fair and 1 failure. In the study conducted by Panchal et al. [53] 15 patients had excellent, 5 had good, 4 had fair and only 1 patient had failure outcome. Similarly in the study conducted by Shriharsha et al. [69] 82 percent cases had excellent/ good outcome, and in the study conducted by Bohra et al. [70] 77.5 percent patients had excellent outcome.
These studies are comparable to our study in which 82 percent of type A fractures had excellent results and 76.9 percent of type C fractures had excellent or good outcome. Similarly excellent results were seen in 16 cases good results in 11 cases satisfactory in 2 cases and failure was seen in 1 case. A study conducted by Bohra et al. [70] showed that only 2 cases had complications of superficial infection [70]. In another study conducted on 2 patients developed superficial infection and 2 patients developed implant discomfort/ tenderness. Similarly in the study conducted by Kiran et al. [62] no cases of infection were reported. Similarly in the study conducted by 2 cases of contracture, 1 case of implant failure and 1 case of residual infection was observed. In our study only 2 patients had superficial infection which was managed with regular dressings and oral antibiotics (cephalexin) for 7 days after sending swab for culture and sensitivity reporting [71-73]. The incidence of infection in our case can be attributed to the fact that open reduction technique was used in our study [74].
The limitations of the study includes that the study was carried out in a single institution in small number of cases, so a large scale study is required to formulate further inference. The long term follow up could not be assessed because of limitation of study period. So long term outcome of the patient could not be assessed in the long run. The need for secondary operation for plate removal has not been discussed in this study due to short follow up time.
Over the years, different treatment options have been proposed for supracondylar femur fracture like conservative management with skeletal traction and surgical management with dynamic condoler screw, retrograde intramedullary nailing, but recently it has been found especially in communities, Intraarticular fractures and osteoporotic people that the functional outcome in these patients is not very good. In this study 30 patients with supracondylar femur fracture were managed with distal femur locking compression plate with good to excellent outcome. The method of treatment is standard with good exposure of fracture fragments, less operative time and good functional and radiological outcome. To conclude, locking compression plate is an important modality in treatment of fractures around knee especially when fracture is severely communities and in situations of osteoporosis.


