Impact Factor : 0.548
- NLM ID: 101723284
- OCoLC: 999826537
- LCCN: 2017202541
Basuki Supartono*
Received: October 15, 2018; Published: October 26, 2018
*Corresponding author: Basuki Supartono, Stem Cell Research and Tissue Engineering Center, Medical Faculty of University Pembangunan Nasional Veteran Jakarta, Indonesia
DOI: 10.26717/BJSTR.2018.10.001960
Diabetic wound is the most dreadful complication of Diabetes Mellitus (DM) in musculoskeletal system of human being. Diabetic wound healing is considerably challenging due to the poor ability of tissue regeneration in diabetic patients. Here we reported a case study of tissue engineering therapy on unhealed wound in the back of young female DM patient. We decided to not do any surgery treatment. We did standard wound therapy with combination tissue engineering therapy. The tissue engineering treatment will be using Peripheral Blood Mononuclear Stem Cells (PBMNCs), Cord Blood Mononuclear Stem Cells (CBMNCs), Collagen, and Plasma Rich Platelets (PRP). To develop a PRP preparation, blood must first be drawn from patient and put it in PRP tube. The platelets are separated from other blood cells and enriched by centrifugation. CBMNCs were isolated from human placenta blood (donor) which is collected during delivery process, the PBMNCs were isolated from patient's blood and they were extracted with Ficoll gradient. PRP and MNCs was applied topically and subcutaneously to the wound. We gave collagen every week, PBMNCs at week 4, CBMNCs at week 6 and PRP at week 8. We did tissue engineering therapy for 8 weeks and the result showed perfect wound healing without complication. In conclusion tissue engineering therapy using MNCs stem cell, PRP and collagen could treat successfully unhealed diabetic wound.
Abbreviations: PBMNCS: Peripheral Blood Mononuclear Stem Cells; CBMNCS: Cord Blood Mononuclear Stem Cells; PRP: Plasma Rich Platelets; DM: Diabetes Mellitus
Diabetes mellitus (DM) often inflicts complication on musculoskeletal system in the form of diabetic wound. This complication is very terrifying because diabetic wound often ends up with amputation and resulted in death. Diabetic wound is difficult to heal despite various interventions such as wound care and surgery has been done. It gives a challenge to clinicians to solve this problem. Generally, wound healing is a complex process and requires good function and integrity of the tissue. The process may be disrupted due to several factors and when it occurred, wound healing process would be disturbed, and wounds are difficult to heal, it becomes severe, chronic wound and ends up with unhealed wound. Several factors that inhibiting wound healing process includes continuous pressure to tissues, blood vessels obstruction, elderly, and chronic diseases such as DM. Diabetic wounds are difficult to heal because the patient has dysregulation in the wound healing process, both in tissue level and cellular level.
In tissue level there are neurological and vascular disorder, also infection. In cellular level there are disturbance in cell proliferation, extracellular matrix production, growth factor expression, and failure of neovascularization. Until now, diabetic wound therapy consists of debridement, wound pressure release, antibiotic administration and blood flow management. The therapy has not been satisfactory yet, therefore a breakthrough is needed to overcome the problem the current therapy had only touched healing process in tissue level, not yet at cellular level. We need cellular based diabetic wound therapy; the alternative is tissue engineering [1]. Tissue engineering is a technique to repair damaged tissues by using three components, i.e. cells, signal molecules and scaffolds. These techniques are comfortable and safe for patients and they give satisfactory results. The cells used were stem cells, and signal molecules used were growth factors. Meanwhile, the scaffolds used were certain media.
Stem cells are cells that has not yet certain shape and function, however they have the ability to renew, replicate, and form new cells and tissues structuring the organism body. Stem cells found in embryo cells are called embryonal stem cells, and they can also be found in body tissues which were called tissue stem cells. Tissue stem cells were obtained by isolating mononuclear cells (MNCs) from tissues such as skin, fat, cord blood, and peripheral blood. Tissue stem cell has regenerative capability, which is the ability to repair itself. This feature has constitutive and facultative characteristics. Constitutive means tissue repair was conducted only when needed and facultative means activation only occurs when there is injured tissue. Other than that, tissue stem cell has plastic characteristics which it can form other cells differently from its lineage [2]. Stem cell can be given through several administration routes, i.e. intravenous injection, intraarticular injection, subcutaneous injection, or topical [1]. Tissue engineering using growth factor as its signal molecule it has been proven to trigger tissue regeneration. Growth factors can be isolated from peripheral blood of patient, namely plasma rich platelets (PRP) [3,4].
Tissue engineering technique also uses scaffolds as media, such as collagen. Tissue engineering technique has been proven very beneficial for banal diabetic wound healing. The author previously used MNCs stem cells without scaffolds and growth factor for diabetic wound healing with satisfactory result [1]. The objective of this article is to report the success of diabetic wound therapy using MNCs stem cells with the addition of scaffolds (collagen) and growth factors (PRP).
The patients were given information and were consented to standard wound therapy in combination with tissue engineering techniques. We received female patient with diabetes mellitus (46 years old) with 6 x 6 cm post-surgical wound on the back with sutures still visible accompanied by infection sign of redness on the sides of the wound. The wound has not healed for 2 months after the first surgery which was the removal of atheroma cyst. Afterwards, wound suture surgery was performed but the wound still had not healed. The patient rejected further surgery from the previous surgeon. The patient continued to routinely visit the internist regarding her diabetes mellitus and consumed antidiabetic medication and antibiotics.
Wound therapy was performed by orthopedic surgeon once a week till 8 weeks. It is carried out by applying the principle of sterility. The solution used to clean the wound were H2O2 solution, NaCl solution, and Povidone Iodine solution. The dead tissues were removed, the wound was cleaned and covered layer by layer with collagen (Collacure, Biot Technology Co., Ltd., China, Indonesian Ministry of Health, AKL 31603711554), tulle (Melladerm® - Plus Tulle SanoMed Manufacturing B.V, Netherlands, Indonesian Ministry of Health, AKL 21603113120), wet gauze, dry gauze, and waterproof plastic (Tegaderm™ Film, 3M Health Care, USA). This layer enables the patient to take shower as usual.
After receiving explanation and signing informed consent, 30 ml of the patient's peripheral blood was taken for MNC stem cells isolation. As many as 100 ml cord blood was taken by obstetrician in sterile room (operating room) after the donor was given explanation and signed informed consent. The blood of the donor was tested to determine infection risk of hepatitis and HIV, and both results were negative. All procedures in taking and examination of blood samples conducted in Al Fauzan Hospital. MNCs were isolated from the blood by using gradient centrifugation principle. Blood specimens were diluted with NaCl sulution, filtrated with Ficoll solution and and rotated in cold centrifugation instrument. Buffy coat layers were taken, washed and supernatant was removed untill only MNC cells available to be counted and viability checked. Isolation result obtained 33 x 105 peripheral blood MNCs with 98% viability, and 40 x 105 cord blood MNCs with 98% viability. The MNCs were made suspension with 5 ml NaCl.
After receiving explanation and signing informed consent, 10 ml of the patient's peripheral blood was taken for PRP isolation. The blood was then inserted to a tube then rotated in centrifugation instrument until PRP was separated from other blood. PRP was taken using special needle.
Application of tissue engineering components was given after the wound has been cleaned. Collagen was given once a week for 8 weeks. MNCs and PRP were given through topical application and subcutaneous injection.
Wound evaluation was performed every visit, once a week. Parameters observed were infection signs, wound fluid production, wound size, granulation tissue and the possibility to perform re surgery.
This therapy provides very satisfying result. The progress of therapy was visible every week and the wound healed completely on the end of week 8. The progression of wound healing was marked by absence of infection signs, decreased wound size, growth of granulation tissue and good wound closure. Until the end of the therapy, there was no indication to perform surgery such as debridement or skin graft [Table 1]. These results proved that tissue engineering therapy using collagen, PRP and MNC stem cells can heal chronic diabetic wound that were previously difficult to heal. For 8 (eight) weeks of therapy, there were no side effects of local or systemic allergic reaction or other complaints. Further details can be seen in the figure (Figure 1 & 2).
Kirana et al., 2012 and Salmeron et al., 2011 reported successful diabetic wound healing using MNC stem cells [1]. Those studies were not similar to our study in the components of tissue engineering, stem cells source, amount and therapy duration.
The authors only used one component which was MNC stem cells without the addition of collagen and growth factors. The stem cells used were derived from aspiration of patient's bone marrow. The collection of this fluid was uncomfortable and risk to the patient. The collection of stem cells from bone marrow was conducted maybe the author needed a lot of cells. However, the amount is not the same as the potential. The author used stem cells in huge amount, which were between 2 60 - 3 00 x 106 cells. Besides, the healing duration was quite long, between 3-13 months. We used blood stem cells with only few amounts but with the addition of collagen and PRP, the results were satisfactory with shorter healing duration. The differences may occur due to the difference in case, which in previous author's case, the diabetic wound was accompanied by vascular disorder.
MNC stem cells healed diabetic wound through various mechanisms, including suppressing inflammatory reaction, increasing growth factor for vascular formation, differentiation of blood cells, fibroblasts, muscle cells, and neuron cells [1].Other than that, MNC stem cells also produce protein which can suppress the activity of infection-causing bacteria [5]. Moreover, MNC stem cells can also suppress the growth of bacteria [6]. The results of this therapy were in accordance with the report of successful diabetic wound healing with peripheral blood stem cells of the patient as seen in the Figures 3 & 4 [1]. MNCs stem cell collection from the blood was more comfortable and safety, therefore the use of blood MNC stem cells (PBMNCs, CBMNCs) is very promising for diabetic wound therapy [7]. However, there was still limitations in this report because of the limited number of cases. Further studies are needed to support scientific basis of the use of stem cells and to answer several questions regarding patient characteristics, donor characteristics, effective dose, parameter of evaluation, effectivity and safety patient. Tissue engineering technique was proven very beneficial for diabetic wound healing in which it was not found its solution before.
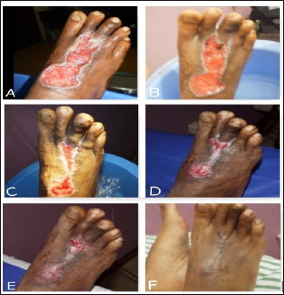
Figure 4: Wound healing progress.
A. The Wound Appearance before PBMNCs administration.
B. After 1st PBMNCs administration.
C. After 2nd administration.
D. After 3rd administration.
E. After 4th administration.
F. After 5th administration or 2 months of treatment, the ulcer is completely healed.
However, the application should consider several things. Use of components should consider medical regulation, legal aspect and patient belief. All of the aspects should be communicated and approved by the patient. There are type of tissue engineering components, which are not alive and alive component. Not alive components include scaffolds and signal molecules in the form of proteins. Scaffols are available in two preparations, i.e. fermentation result of certain bacterial cells or isolation result of animal tissue. There are natural and synthetic signal molecules, and there are molecules isolated from human blood. The researcher should choose good quality of scaffolds and signal molecules which are in accordance with patient belief. Alive component is stem cell with all of its living properties. The use of stem cell should consider several things, i.e. donor, the type of material and delivery method. Stem cells donor can be derived from animal or human. Human stem cells can be auto log or allograft. The type of stem cells transplanted can use embryonal stem cells or tissue stem cells such as MNC stem cells. The researcher should choose stem cells that is legal, good quality and in accordance with the patient s belief.
In conclusion, tissue engineering therapy using HCBMNCs, HPBMNCs, and PRP could successfully treated unhealed diabetic wound.
We thank for Prita Kusumaningsih MD, Obstetric and Gynaecologic Specialist, Muzayyana Sakiinah MD, Ns. Latifah, Khurnia Safitri and all of the Staff of Al Fauzan Hospital for invaluable help in this research.


