Abstract
Acute abdomen in women of childbearing age is a clinical presentation that requires emergency surgical treatment in many cases and rapid diagnosis is oftentimes essential. Most are the causes of acute abdomen: gynecological (ectopic pregnancy, ovarian torsion, ovarian cysts, endometriosis, pelvic inflammatory disease) and non-gynecological (appendicitis, Crohn’s disease, Meckel’s diverticulitis, sigmoid diverticulitis, perforated peptic ulcer, viral gastroenteritis, hernias, urological disease). Appendicitis and pelvic inflammatory disease (PID) are two of the most common causes of abdominal pain in women of childbearing age. This article is a systematic review of literature of the differential diagnosis between appendicitis and PID. The diagnosis is clinical, laboratory and radiological. When the sign and symptoms and the biochemical markers are nonspecific abdominal ultrasound (US) is the first radiological test that is performed, but the computer tomography (CT) remains the best specific and sensible exam for the differential diagnosis. Nuclear Magnetic Resonance is performed when CT is contraindicated. Other test like transvaginal ultrasound is a relatively simple and inexpensive diagnostic test that could easily complement the classic abdominal US and be part of the routine diagnostic protocol of women with acute abdominal pain. Therefore, a careful management of the patient starting from the clinical examination and passing through the laboratory and radiological characteristics is necessary.
Keywords: Acute Abdomen; Right Acute Abdomen; Appendicitis; Pelvic Inflammatory Disease; Women of Childbearing Age
Abbreviations:US: Ultrasound; CT: Computer Tomography; CRP: C-Reactive Protein; AIR: Appendicitis Inflammatory Response; AAS: Adult Appendicitis Score; PID: Pelvic Inflammatory Disease; PMN: Polymorphonuclear; NAATs: Nucleic Acid Amplification Tests
Introduction
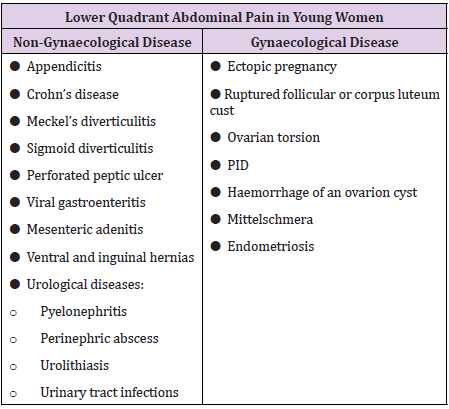
Acute abdomen is a clinical presentation that requires emergency surgical treatment in many cases, rapid diagnosis is oftentimes essential. The diagnoses associated with an acute abdomen vary according to age and gender [1], and it is more difficult in young women, in which it is necessary to distinguish between gynecological and non-gynecological diseases (Table 1). Non-gynecological causes include appendicitis, which remains one of the main causes of acute abdomen in childbearing women. The diagnosis of acute appendicitis is essentially clinical. Appendicitis can initially present with periumbilical pain that migrates to the right lower quadrant, classically more intense over McBurney’s point. The pain can be associated with fevers along with nausea, vomiting and anorexia, that classically occur after pain onset. Common laboratory abnormalities include leukocytosis (white blood cells WBS > 20.000 cells/mm3) and an elevated C-reactive protein (CRP) level. Although appendicitis is a highly prevalent disease, especially in Western countries, diagnosis remains a challenge for the surgeon and requires a combination of medical history, laboratory tests, clinical and diagnostic imaging (ultrasound, CT and MRI). Several clinical and laboratory-based scoring systems have been devised to assist diagnosis and the most widely used are the Alvarado score, the AIR (Appendicitis Inflammatory Response) and the AAS (Adult Appendicitis Score).
The last WSES guidelines [2] on appendicitis recommend the use of AIR score and AAS score as clinical predictors of acute appendicitis (Table 2). In women of childbearing age, the diagnosis is further complicated because, in case of lower abdominal pain, appendicitis must be distinguished from a variety of gynecological conditions in order to avoid unnecessary intervention. A careful gynecological history should be taken in all women with acute abdomen, concentrating on menstrual cycle, vaginal discharge and possible pregnancy. For all female patients of childbearing age, pregnancy testing should always be part of the workup for any abdominal pain to rule out ectopic pregnancy. Other gynecologic causes include ruptured ovarian cysts, mittelschmerz (midcycle pain occurring with ovulation), endometriosis, ovarian torsion, ectopic pregnancy and pelvic inflammatory disease (PID) [3,4]. PID comprises a spectrum of diseases that include salpingitis, endometritis and tubo-ovarian sepsis. Typically, the pain is lower intense than in appendicitis and is bilateral. A history of vaginal discharge, dysmenorrhea and burning pain on micturition is a helpful differential diagnostic point. The physical findings include cervical tenderness on vaginal examination. When suspected, a high vaginal swab for Chlamydia trachomatis and Neisseria gonorrhoeae culture should be taken and a transvaginal ultrasound can be performed.
Treatment is usually a combination of ofloxacin and
metronidazole for 14 days. The diagnosis of PID is both difficult
and important as more than 60% of women who have severe PID
or multiple PID episodes become infertile. In addition, missed
or delayed diagnosis are associated with chronic pelvic pain and
ectopic pregnancy [5,6]. Appendicitis and pelvic inflammatory
disease (PID) are two of the most common causes of abdominal
pain in women of childbearing age [7]. The estimated prevalence
of self-reported lifetime PID was 4.4% in sexually experienced
women of reproductive age (18-44 years) in the US. Based on
NHANES 2013-2014 data, an estimated 2.5 million women aged
18-44 years in the United States reported a lifetime history of PID
diagnosis. Nevertheless, in the United States, 250,000 cases of
appendicitis are reported annually, representing 1 million patient days of admission and occurs in 7% of the US population, with an
incidence of 1.1 cases per 1000 people per year [8]. Due to the
similar presentations of these conditions, the rate of misdiagnosis
is high. In fact, the most frequent reason for malpractice claims
against emergency department physicians is missed appendicitis
diagnosis. It is important to be vigilant evaluating and treating
women at risk for appendicitis and PID because the sequelae of
either condition left untreated can be as severe as death.
The aim of this article is to review the literature to identify the
criteria to distinguish appendicitis from PID, to make an earliest
possible diagnosis and treatment.
Material and Methods
We conducted a review of the PubMed database searching the terms “appendicitis” and “pelvic inflammatory disease OR PID” in publications from 2000 to 2021 and filtering the results by population of women of childbearing age (13-44 years). Our search showed 95 results. After analyzing the scientific articles, we extrapolated 26.
Results
Clinical Diagnosis
Abdominal pain in women of childbearing age can be difficult to
diagnose. In attempting to differentiate appendicitis from PID, many
aspects of history, physical examination and clinical data can help to
clarify the diagnosis. However, some of the data historically used in
differentiating appendicitis and PID have not proven to be useful in
studies. Women of childbearing age who go to the emergency room
for acute abdominal pain usually have various symptoms that can
direct the diagnosis towards a gynecological or intestinal pathology.
It is usually difficult to distinguish acute appendicitis from PID just
based on the patient’s clinical examination during the first visit.
Various studies have analyzed aspects of differential diagnosis
between the two diseases. Charveriat, et al. [9] concluded that
adnexal pain resulting from cervical motility is the most important
clinical sign of PID (sensitivity 95-99%) and may be associated
with other symptoms such as fever, leucorrhea and metrorrhagia
that support the first diagnostic suspicion. Therefore, a patient with
such symptoms should be directed to a gynecological consultation
and a thorough pelvic examination.
Furthermore, a positive history for sexually transmitted
diseases must be investigated to support the diagnosis of PID (with
a specificity of 82%). Other authors [10] consider mandatory for a
woman of childbearing age with non-specific abdominal symptoms
to routinely perform both a complete abdominal examination and a
pelvic-gynecological examination. Kruska [11] in 2010 summarized
the symptoms of PID and acute appendicitis. Positive predictive
values ratio for acute appendicitis were 8.4 for pain in the right iliac
fossa, 3.6 for pain migrating from the periumbilical region to right
iliac fossa, 3.2 for fever and psoas sign, and only 2.0 for positive
Blumberg sign. Regarding PID, leucorrhea (positive predictive value
3,3) and bilateral pelvic abdominal pain (2,5) were very important,
while fever and leukocytosis were less specific. Dahlberg, et al. [12]
specifically analyzed the clinical presentations of the two diseases
and documented that although cervical and uterine pain are more
specific in PID, they are still present in 28% of women with acute
appendicitis. Furthermore, almost 50% of the women who had an
intraoperative diagnosis of acute appendicitis did not present the
classic symptoms of the disease [13]. However, another study point
out that cervical motion tenderness alone is not specific for PID;
it is present in 25% of cases of appendicitis and 50% of ectopic
pregnancies.
Morishita study in 2007 [14] is the most relevant on the clinical
presentation of these two pathologies. In this retrospective study,
the data of 181 women with abdominal pain were analyzed, 109 with
appendicitis diagnosis and 72 with PID. The authors demonstrated
that women with PID were younger (p = 0.003), with a higher body
temperature (p = 0.016), with bilateral pelvic pain (p <0.001), and
with cervical motility pain (p <0.001). Contrariwise, women with
acute appendicitis had more epigastric pain (p <0.001), migrating
pain (p <0.001), appetite loss (p <0.001), nausea and vomiting (p
<0.001) and right iliac fossa pain (p < 0.001). Other studies have
focused their attention on the need of further radiological and
clinical investigations to distinguish PID from acute appendicitis
because the clinical examination alone is not sufficient for the
correct diagnostic classification. Moreover, Dahlberg, et al. [12]
analyzed the patient’s number of pain episodes and their duration.
Typically, an acute onset pain is associated with appendicitis than
PID. Acute appendicitis’ pain usually lasts 24 to 36 hours, while the
pain of PID can last for weeks or until treated. It is clear how the
clinic itself can direct the surgeon towards a differential diagnosis
between PID and acute appendicitis in women of childbearing age,
but it must be accompanied by further laboratory and radiological
investigations.
Laboratory Diagnosis
All women of childbearing age who present to the emergency
room with acute abdominal pain undergo a blood sample for
routine blood chemistry tests. These consist of blood counts with
leukocyte formula, liver function tests, renal function tests and
measurement of inflammation markers (for example erythrocyte
sedimentation rate and CRP). Furthermore, if the painful symptoms
affect the lower quadrants of the abdomen, a chemical-physical
examination of the urine could be performed [15]. From the studies
published on this topic, the simple execution of routine blood
tests does not allow us to differentiate PID and acute appendicitis
because an increase of inflammation indices (white blood cell
counts and elevated CRP) is possible in both clinical conditions.
In case of prolonged observation of the patient, it may be useful to repeat the routine blood tests because a rapid worsening of the
indexes of inflammation can highlight an acute appendicitis rather
than a PID [12].
In patients of childbearing age with abdominal pain, a b-hcg
test should be always done to exclude an unrecognized or ectopic
pregnancy [12]. Second level examinations may be useful in
patients with non-specific abdominal symptoms. Among these,
certainly important is a cervical swab to diagnose genital infections
(for example Neisseria gonorrhoeae or Chlamydia trachomatis)
which would support the diagnosis of PID. The findings of 10 or
more polymorphonuclear (PMN) leukocytes on a gram-stained
endocervical smear is diagnostic of mucopurulent cervicitis and can
help substantiate the diagnosis of PID. Rapid tests for the detection
of these microorganisms are available [11]. Most physicians are
now using nucleic acid amplification tests (NAATs) to detect
chlamydia and gonorrhea. These tests amplify and detect DNA
and RNA sequences and are much more sensitive than previous
chlamydia and gonorrhea tests. Urine NAATs have sensitivities and
specificities like those of cervical samples [12].
Newer evidence documents that microorganisms associated with bacterial vaginosis have been found in women with laparoscopically proven PID. However, it is important to realize that the sensitivity of the clinical diagnosis for PID based on a pelvic examination alone is only 60% to 70%. Considering additional biochemical markers that may aid in the differential diagnosis between PID and acute appendicitis, some authors have considered intrauterine nitric oxide measurement [16]. In this retrospective case-control study, intrauterine nitric oxide (NO) values were compared in women with a laparoscopic diagnosis of appendicitis or PID. In patients with PID, NO values were found much higher than those with appendicitis or compared to healthy controls. Other biochemical markers of inflammation like interleukin-6, IL-8 and CD-64 have been associated with appendicitis compared with nonsurgical causes of acute abdominal pain [17]. On the contrary the plasma levels of LRG1 were not useful to differentiate between acute appendicitis and pelvic inflammatory disease [18].
Radiological Diagnosis
All women who come to the emergency room for acute abdominal pain undergo to first-level radiological investigations [19,20]. Among these, the first is abdominal ultrasound (US). This gives informations about the presence of free abdominal fluid, free air, intestinal obstruction, parenchymal pathologies (hepatic, splenic, renal, adrenal, pancreatic), appendicular and gynecological pathologies or conditions (adnexal cysts, ovarian torsions, pelvic abscesses, uterine fibroids, etc.) and vascular diseases (aneurysms or arterial dissection).
Abdominal Ultrasound (US)
In the differential diagnosis between PID and acute appendicitis, abdominal ultrasound can guide the diagnosis but, in some cases, this is not diagnostic because both clinical conditions may have similar presentation (fluid in Douglas and ovaries, salpingi and appendix edematous and thickened) [21]. Therefore, in women of childbearing age with doubtful diagnosis it is always indicated to perform a gynecological examination with transvaginal ultrasound that permit a more accurate visualization of the adnexa and the uterus. Other studies [22,23] have shown that ultrasound, in the diagnosis of acute appendicitis, has a sensitivity of 75-90% and specificity of 85-98% with the advantages of a lack of ionizing radiation and a high positive predictive value (95%). The normal appendix is rarely seen by US. Usually, the ultrasound presentation corresponds to an edematous appendix with thickened walls, with a periappendicular fluid flap and, in the most severe cases, periappendicular air bubbles or free abdominal air. Nevertheless, the diagnosis of acute appendicitis can be made by demonstration of a non- compressible, aperistaltic, blind-ending tubular structure measuring greater than 6 mm in diameter. The periappendiceal fat may be echogenic due to the inflammation, and color doppler US may be helpful in showing hyperemia within the thickened wall [24].
Some findings, such as submucosal ring, echogenic fat and intraluminal gas are always absent in acute PID. Similarly, cogwheel sign or incomplete septum were not observed in appendicitis [23]. Difficulties in diagnosis occur if there is a true retrocecal appendix, if the inflammation is limited to the tip of the appendix, if gas in the appendix makes it difficult to differentiate from terminal ileum, and in perforation when the appendix decompresses effectively destroying the most important sonographic feature. Secondary findings then become necessary to assist diagnosis and include loculated pericecal fluid, thickening of adjacent bowel walls, thickening and increased echogenicity in the adjacent mesentery or omentum, and frank abscess formation. However, these latter findings are not specific for appendicitis and can be seen with other intraabdominal inflammatory processes [23]. Moreover, PID tends to be a bilateral process and sonographic features are variable related to the extent of the disease. Endometrial thickening or fluid in the appropriate clinical setting is supportive of an endometritis. Purulent fluid accumulating in the pouch of Douglas in more extensive disease can be identified sonographically as particulate fluid. Salpingitis with tubal occlusion may result in a pyosalpinx.
Computer Tomography (CT)
When the clinical presentation is non-specific and the ultrasound is non-diagnostic, patients undergo abdomen computer tomography (CT) with contrast medium [19,20,22]. The use of CT, which is the test of choice for suspected appendicitis in adults, has been shown to improve diagnostic accuracy. CT decreases the falsenegative rate to 4% overall and 8.3% in females of childbearing age. Findings on CT are overall swelling (>6mm), wall thickening, and enhancement of the appendix. Secondary signs include periappendiceal fat stranding, pericolic fluid, and focal thickening of the cecum. The appendix may be difficult to visualize in cases of appendiceal rupture, which may be suspected if there is a focal defect in the wall of the inflamed appendix, an appendicolith outside the appendix, a periappendiceal fluid collection, or extraluminal gas near the appendix [20]. In Hentour’s retrospective study of the role of CT in the differential diagnosis between PID and acute appendicitis, it was found that only two CT findings (appendiceal diameter and left tubal thickening) were very accurate in differentiating PID from acute appendicitis.
Consequently, the first step in interpreting abdominopelvic CT in non-appendectomised women of reproductive age with acute lower abdominal pain is to measure the appendiceal diameter. If the appendiceal diameter is < 7 mm, appendicitis is very improbable and thus CT findings of PID should be investigated. If the appendiceal diameter is ≥ 7 mm, left tubal thickening should be analyzed, since a left tubal diameter ≥ 10 mm would indicate PID rather than appendicitis [22]. Conversely, it has been shown that in PID the most present CT radiological features are haziness of the pelvic fat, obscuration of the pelvic fascial planes, thickening of the uterosacral ligaments, abnormal endometrial enhancement with fluid in the endometrial cavity, enhancement and thickening of the fallopian tubes, and abnormal enhancement, enlargement, and reactive polycystic change of the ovaries [25]. Moreover, the presence of an appendicolith, cecal origin of the tubular structure, and the presence of cecal wall thickening (“cecal bar” sign) are helpful distinguishing features of appendicitis [22]. The sensitivity of CT in appendicitis is from 87% to 98%, higher than US o MRI.
Nuclear Magnetic Resonance (NMR)
In some centers, especially in the United States, the use in
emergency of nuclear magnetic resonance (NMR) has become
routine in the management of acute abdominal pain in women
of childbearing age and in pregnant women [26,27]. Magnetic
Resonance Image (MRI) is a valuable tool in the evaluation of
suspected appendicitis, either as an adjunct to or a replacement
for an initial right lower quadrant US. This is particularly true
for pediatric and pregnant patients, in whom ionizing radiation
must be avoided. Scan times have been decreased using protocols
including as few as four sequences, which allow for diagnostic
imaging of the abdomen and pelvis in almost 15 minutes [21]. MRI
has sensitivity, specificity, and accuracy for diagnosis of appendicitis
of 95%, 89%, and 93%, respectively. For diagnosis of appendiceal
perforation, MRI imaging demonstrates slightly higher sensitivity (57%) than ultrasound with conditional CT (48% sensitivity) [22].
The inflammation will be depicted best on the fluid-sensitive T2-
weighted images; fat saturation allows the signal abnormality to be
more readily apparent. Appendiceal wall thickening (>2mm) will
show hypointense signal on T1-weighted images and hyperintensity
on T2-weighted images, with the caliber of the appendix measuring
greater than 6 mm.
Periappendiceal fat inflammation will manifest as hyperintense
T2 signal, consistent with edema. In the nonpregnant patient,
gadolinium contrast administration increases the sensitivity of MRI
in diagnosing acute appendicitis where intense appendiceal wall
enhancement is seen on the fat-suppressed postcontrast T1 images
[28]. MRI imaging, given the lack of a radiation-associated risk
and the relative safety of gadolinium- based contrast agents, is an
attractive alternative to CT for the evaluation of pelvic inflammatory
disease. Compared with US, MRI imaging provides superior
depiction of adnexal edema. T2-weighted fat-saturated images
show parametrial signal hyperintensity due to edema. A tuboovarian
abscess appears with mild signal hyperintensity on T1-
weighted images and high signal intensity on T2-weighted images
be- cause of internal debris. At contrast-enhanced MR imaging, an
abscess has a thick enhancing wall. Occasionally, an adjacent fluidfilled
tubular structure, which represents an inflamed fallopian
tube, is seen: hydrosalpinx, which may manifest with acute lower
abdominal pain, is well depicted at MR imaging.
Discussion
PID and acute appendicitis remain two frequent pathologies
in women of childbearing age and for this reason many studies
have been performed on this topic. The differential diagnosis
between the two pathologies may not be easy, especially in vague
clinical presentation and with doubtful symptoms. The general
surgeon must pay attention to the possible non-intestinal causes
of acute abdominal pain in young women, also excluding all those
gynecological causes that can mimic acute appendicitis. Studies
have shown that in these patients a complete physical examination
must always include a gynecological examination with cervicovaginal
swabs to look for possible infections. Furthermore, an
adequate sexual history should always be investigated as well as
the use of intrauterine devices that can cause PID. The most recent
studies have shown how a careful clinical analysis, before laboratory
and radiological tests, can guide towards the right diagnosis. Pain
migration from periumbilical to right iliac fossa with positive
Blumberg’s sign is more pathognomonic of acute appendicitis than
bilateral pain, lasting more than 24-36 hours and characterized by
non-worsening that are more specific in PID.
Routine laboratory investigations (complete blood count,
leukocyte count, CRP, erythrocyte sedimentation rate) do not
help to define a correct diagnosis because they are non-specific indicators of inflammation. Microbiological investigations would
be more appropriate to investigate sexually transmitted infections
(Neisseria gonorrhea, Chlamydia tracomatis) in young women with
non-specific abdominal symptoms. More specific laboratory tests
such as the search for inflammatory interleukins 6 and 8 or the
measurement of intrauterine nitric oxide levels appear to be too
specific investigations to be part of routine clinical practice and
should be reserved within study protocols. Among the radiological
investigations, ultrasound is certainly the first diagnostic step in
young women of childbearing age with acute abdominal pain. This
easily gives information in severe clinical presentation of abdominal
pathology but is unfortunately little diagnostic in ambiguous cases
with non-specific symptoms. CT appears to be the most specific
and sensitive diagnostic test, with the best diagnostic accuracy in
distinguishing between PID and acute appendicitis.
However, it should be avoided in children and pregnant women.
CT images have the advantage of defining the characteristics of PID
and acute appendicitis more specifically. The dimensional cut-off
on the thickness of the appendicular walls of 6-7 mm is universally
accepted as a pathognomonic finding of acute appendicitis. As well as
the thickening of the uterosacral ligaments, abnormal endometrial
enhancement with fluid in the endometrial cavity, enhancement
and thickening of the fallopian tubes, and abnormal enhancement,
enlargement, and reactive polycystic change of the ovaries are
more specific radiological signs in PID. MRI plays a secondary
role because it can be rarely performed in emergency, except in
hospitals with great economic and technological resources. The
advantage is no exposition to radiation of patients and excellent
specificity and sensitivity in best defining acute appendicitis or
PID. However, it should be reserved for specific population groups
(pregnant women, children).
On the other hand, transvaginal ultrasound is a relatively simple
and inexpensive diagnostic test that could easily complement the
classic abdominal US and be part of the routine diagnostic protocol
of women with acute abdominal pain. This radiological test has good
sensitivity and specificity to exclude acute appendicitis in those
cases where the gynecological cause of pain is more likely. Certainly,
new and further studies are needed to define the best diagnostic
protocol in women of childbearing age with acute abdominal pain
presenting in ED. Above all, prospective multicenter studies or
randomized trials would be needed.
Conclusion
PID and acute appendicitis are two very frequent pathologies in women of childbearing age. A correct differential diagnosis may not always be easy, especially in not typically clinical presentation. Therefore, a careful management of the patient starting from the clinical examination and passing through the laboratory and radiological characteristics is necessary. A correct diagnosis allows a better patient management and reduction of unnecessary surgeries.
References
- LG Graff IV, D Robinson (2001) Abdominal pain and emergency department evaluation. Emergency Medicine Clinics of North America 19(1): 123-136.
- S Di Saverio, Podda M, De Simone B, Ceresoli M, Augustin G, et al. (2020) Diagnosis and treatment of acute appendicitis: 2020 update of the WSES Jerusalem guidelines. World Journal of Emergency Surgery 15(1): 27.
- Prystowsky JB, Pugh CM, Nagle AP (2005) Appendicitis. Current Problems in Surgery 42(10): 694-742.
- Silen W, Cope Z (2010) Cope’s Early Diagnosis of the Acute Abdomen. Oxford University Press, United Kingdom.
- Weström L (1980) Incidence, prevalence, and trends of acute pelvic inflammatory disease and its consequences in industrialized countries. American Journal of Obstetrics and Gynecology 138(7) 880-892.
- Westrom L, Bengtsson LP, Mardh PA (1981) Incidence, trends, and risks of ectopic pregnancy in a population of women. BMJ 282(6257): 15-18.
- (2017) Prevalence of Pelvic Inflammatory Disease in Sexually Experienced Women of Reproductive Age-United States, 2013-2014. Annals of Emergency Medicine 70(1): 28-30.
- Craig S (2021) Appendicitis: Practice Essentials, Background, Anatomy. Medscape.
- Charvériat A, Fritel X (2019) Diagnostic d’une infection génitale haute : critères cliniques, paracliniques, imagerie, et cœlioscopie. RPC infections génitales hautes CNGOF et SPILF. Gynécologie Obstétrique Fertilité & Sénologie 47(5): 404-408.
- Lloyd TDR, Malin G, Pugsley H, Garcea A, Garcea G, et al. (2006) Women presenting with lower abdominal pain: A missed opportunity for chlamydia screening?. The Surgeon 4(1): 15-19.
- Kruszka P, Kruszka SJ (2021) Evaluation of Acute Pelvic Pain in Women. American Family Physician 82(2): 141-147.
- Dahlberg DL, Lee C, Fenlon T, Willoughby D (2004) Differential diagnosis of abdominal pain in women of childbearing age. Appendicitis or pelvic inflammatory.
- Amit K Bhavsar, Gelner EJ, Shorma T (2021) Common Questions About the Evaluation of Acute Pelvic Pain - PubMed. American family physician 93(1).
- Morishita K, Gushimiyagi M, Hashiguchi M, Stein GH, Tokuda Y (2007) Clinical prediction rule to distinguish pelvic inflammatory disease from acute appendicitis in women of childbearing age. The American Journal of Emergency Medicine 25(2): 152-157.
- Reust CE, Williams A (2021) Acute Abdominal Pain in Children – PubMed, American family physician 93(10).
- Sioutas A, Ehrén I, Lundberg JO, Wiklund NP, Gemzell-Danielsson (2008) Intrauterine nitric oxide in pelvic inflammatory disease. Fertility and Sterility 89(4): 948-952.
- Saito JM (2012) Beyond appendicitis. Current Opinion in Pediatrics 24(3): 357-364.
- Lontra MB, Savaris RF, Cavazzola LT, Maissiat J (2021) Comparison of leucine-rich alpha-2-glycoprotein-1 (LRG-1) plasma levels between patients with and without appendicitis, a case-controlled study. Scientific Reports 11(1).
- Heiken JP, Katz DS, Menu Y (2021) Emergency Radiology of the Abdomen and Pelvis: Imaging of the Non-traumatic and Traumatic Acute Abdomen. IDKD Springer Series: 123-143.
- El Hentour K, Millet I, Pages Bouic E, Curros Doyon F, Molinari N, et al. (2017) How to differentiate acute pelvic inflammatory disease from acute appendicitis? A decision tree based on CT findings. European Radiology 28 (2): 673-682.
- Wongwaisayawan S, Kaewlai R, Dattwyler M, Abujudeh HH, Singh AK (2016) Magnetic Resonance of Pelvic and Gastrointestinal Emergencies. Magnetic Resonance Imaging Clinics of North America 24(2): 419-431.
- Vandermeermd FQ, Wong You Cheong JJ (2010) Imaging of Acute Pelvic Pain. Topics in Magnetic Resonance Imaging 21 (4): 201-211.
- Sivyer P (2000) Pelvic Ultrasound in Women. World Journal of Surgery 24(2): 188-197.
- Molander MVP, Paavonen J, Sjöberg J, Savelli L, Cacciatore B (2002) Transvaginal sonography in the diagnosis of acute appendicitis. Ultrasound in Obstetrics and Gynecology 20(5): 496-501.
- Revzin, Mathur M, Dave HB, Macer ML, Spektor M (2016) Pelvic Inflammatory Disease: Multimodality Imaging Approach with Clinical-Pathologic Correlation. RadioGraphics 36(5): 1579-1596.
- Byott S, Harris I (2016) Rapid acquisition axial and coronal T2 HASTE MR in the evaluation of acute abdominal pain. European Journal of Radiology 85(1): 286-290.
- Mervak BM, Wilson SB, Handly BD, Altun E, Burke LM (2019) MRI of acute appendicitis. Journal of Magnetic Resonance Imaging 50(5): 1367-1376.
- Singh A, Danrad R, Hahn PF, Blake MA, Mueller PR, et al. (2007) MR Imaging of the Acute Abdomen and Pelvis: Acute Appendicitis and Beyond. RadioGraphics 27(5): 1419-1431.

 Review Article
Review Article