ABSTRACT
Objectives: To understand the recovery of consciousness among patients following
painless induced abortion under anesthesia and analgesia using propofol and sufentanil
as well as to explore the optimal in-hospital observation period.
Methods: A questionnaire was used to investigate memory, orientation, excitability,
motor coordination and sense of fatigue after induced abortion under anesthesia and
analgesia using propofol and sufentanil.
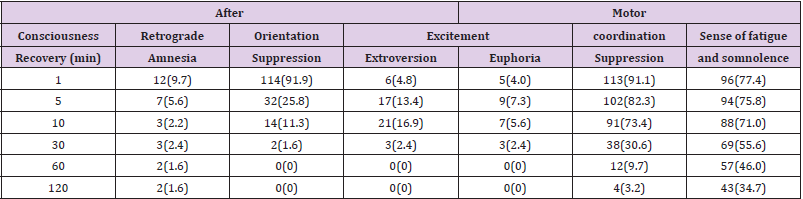
Results: 1.6% of patients had retrograde amnesia 2h after operation. Some patients
showed increased excitability and had a sense of well-being within 30 min after the
operation began. Orientation was affected for 1 to 30 minutes, while decreased motor
coordination and a sense of fatigue might last for 2h after the operation.
Conclusion: Although patients quickly regained full consciousness after induced
abortion under anesthesia and analgesia using propofol and sufentanil, memory,
excitability and motor coordination were unable to recover to preoperative levels and
were accompanied by disorientation and a sense of fatigue. A routine 30-minutes clinical
observation period is not appropriate for all patients. The in-hospital observation
period should depend on individual patient response to drugs and whether the patient
is accompanied by others to ensure personal safety.
Synopsis: The in-hospital observation period following painless induced abortion
should depend on patient response to drugs and availability of others to ensure patient
personal safety.
Keywords: Induced Abortion; Out-patient; Propofol; Sufentanil; Consciousness; Safety
Abbreviations: BP: Blood Pressure; ECG: Electrocardiogram; SPO2: Pulse Oxygen Saturation; HR: Heart Rate
Short Communication
In clinical painless induced abortion, it is obligatory that patients who do not suffer any operative pain or special discomfort should regain consciousness completely within a short time after the operation, return to their preoperative state and leave the hospital safely. Intravenous anesthesia using propofol and sufentanil has been widely used in painless induced abortion [1]. It is characterized by precise anesthetic effect, quick onset and quick elimination without significant accumulation. Patients regain consciousness completely and have no memory of the operation. It can inhibit the vagus reflex and eliminate the induced abortion syndrome, has minimal affect on circulation and respiration and is relatively safe [2]. However, dosage is frequently excessive or insufficient. Excessive dosage will delay recovery and insufficient dosage will affect the operation [3]. At present there is still no domestic uniform standard for the retention and in-hospital observation time for patients following induced abortion. In this article we carried out a survey of patient recovery of consciousness following induced abortion to provide criteria for the safe discharge of patients with relationship to their state of wakefulness.
Materials and Methods
There is no uniform standard for in-hospital observation of patients after induced abortion under anesthesia and analgesia using propofol and sufentanil. In this article, we surveyed the recovery of consciousness of patients following induced abortion to provide evidence for clinical use. One hundred and twenty four patients who volunteered for the questionnaire were at ASA I grade, with an average age of 25.8±5.6 years, weight of 58.8±9.6kg and gestation period of 63±11.6 days. With fasting and water deprivation for 12h before operation, the blood pressure (BP), electrocardiogram (ECG) and pulse oxygen saturation (SPO2) was continuously monitored in the operation room. Beginning three min before the operation, atropine 0.5 mg, 0.15ug/kg sufentanil and 2mg/kg propofol was given in succession by intravenous injection within 2 min, respectively. When patient consciousness and eyelash reflex were no longer present, the operation began. BP, heart rate (HR) and SPO2 were recorded before the anesthesia, 1 min, 2 min, 5 min, and 10 min after anesthesia and observations were made to determine any adverse reactions. The doctor filled out the unified tabular questionnaire after questioning patients. Consciousness recovery:
Retrograde Amnesia
Before the operation, patients were shown two pictures of familiar animals (dog and cat) and then asked to distinguish these among five pictures after the operation.
Orientation
Determination was made whether patients could tell the direction indicated by doctors.
Excitability
Whether the patient took the initiative in communicating with medical staff or other patients.
Motor coordination
While standing or walking, whether patient’s step was sure.
Fatigue
Whether the patient had a sense of fatigue or drowsiness. Data was statistically processed by Excel 2003. Measurement data were expressed withx ±SD using t-test.
Results
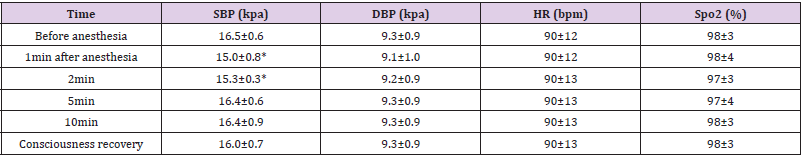
The systolic pressure decreased one and two min after anesthesia, a statistically significant difference compared with that before anesthesia (P <0.05). However, for patients without severe hypotension who needed ephedrine, there was no statistical difference in systolic pressure at other time points compared with that before anesthesia (P <0.05). There was no statistical difference in diastolic pressure, heart rate or blood oxygen saturation before or after anesthesia (P <0.05) Table 1. Eighty-nine (71.8%), 28 (22.6%) and 12 (9.7%) patients had adverse reactions of respiratory depression, injection pain and postoperative nausea, respectively. The respiratory cases showed lower respiratory frequency and apnea with a period of 36±15.8s after intravenous injection of propofol. It took the patients 3.8±1.4min to regain consciousness. Some patients had retrograde amnesia. The orientation suppression and increased excitability lasted 30 min after the operation, while motor coordination suppression and sense of fatigue lasted 2h after the operation Table 2.
Table 1: Changes in Patient Vital Signs before and after Anesthesia ( X ±S).
Note: Compared with that before anesthesia *P<0.05.
Discussion
In this group, patient systolic pressure was significantly
decreased one and two min after the administration of drugs,
which, however was within the normal range and did not
significantly affect their recovery of consciousness, with no need
for special treatment. It is common knowledge that an intravenous
injection of propofol and sufentanil will cause apnea in most
patients and so in administering anesthesia it is necessary to use
auxiliary respiratory measures before hypoxia occurs [4,5]. Thus
hypoxia had no influence on the recovery of consciousness in this
group of cases with a blood oxygen saturation of < 96% [6]. After
an intravenous injection of propofol, patients became unconscious
with the disappearance of the eyelash reflex and respiration
response. The inability to remember the operation is not amnesia.
Retrograde amnesia within the initial 5 min following recovery of
consciousness might be related to incomplete consciousness [7],
but 2h later 1.6% of patients still did not have full preoperative
recall, which might be relevant to propofol.
Wang Chunyan [8] thought patients undergoing non-cardiac
surgery just after a general anesthesia had cognitive functional
disorder. Simon [9] also thought that patients had preoperative
retrograde amnesia after propofol anesthesia. As reported in
most literature, propofol is not stimulatory [10]. However, it was
discovered that in our target group, after regaining consciousness,
patients experienced a definite degree of excitability. Different from
hallucination or nightmare caused by ketamine, this was a feeling
of comfort and pleasure lasting for 5 to 30 min, which expressed
itself among some patients who had not liked communicating
with others before the operation in that they actively began to talk
about how good they felt after the operation. Individual patients
displayed initiative in describing their own dreams and a few
patients involuntarily swung their legs back and forth, seeming
to forget they were in an operating environment. Finco G, et al.
[11] also discovered that patients had a sense of well-being after
gastroscopy and propofol anesthesia but did not analyze this.
Dizziness and disorientation appeared for a certain period of time
after the operation, but patients basically recovered within 10 min.
This is similar to the observed results of Bouillon T, et al. [12].
But in the present study, we also discovered that the
disorientation of a very few patients (1.6%) continued at some
level 30 min after operation. The decrease in motor coordination
was mainly manifested as wobbling as patients walked immediately
after operation. Sometimes patients themselves described this as
“weakness of legs.” In our observation, 2 patients nearly fell while
walking, which was considered related to propofol and sufentanil.
There were also reports of dizziness even with a single use of
propofol [13]. As an opioid drug, sufentanil’s above-mentioned
side effects were clearly in evidence. Currently there are no unified
regulations concerning postoperative management for painless
induced abortion using propofol and sufentanil [14].
In most hospitals, patients are kept under observation for
30 min, while some hospitals, especially small hospitals, don’t
even have an observation room at all. Although an increase in
postoperative excitement is transient, it is inappropriate for
patients to leave the hospital too early due to the patient’s decreased
safety awareness. Because orientation and motor coordination
are affected, patients might fall or even hurt themselves if they
began to walk alone immediately after the operation. Generally,
patients have a sense of fatigue and some even have drowsiness.
In our investigation, it was also discovered that a very few number
of patients were not accompanied by family members or even
returned home by themselves on bicycle after the operation due
to insufficient awareness of the safety issues surrounding painless
induced abortion.
The doctor should give patients safety instructions and explain
to them preoperative fasting and water deprivation, the need to
be accompanied by others and the prohibition against driving.
Patients should be accompanied by nurses back to the observation
room instead of walking alone immediately after operation. It
is advisable that patients without nausea or vomiting after the
operation take fluids or soft food, while fluid infusion may be considered for patients with a poor constitution who cannot eat
[15]. In our hospital, an observation period of 30 to 120 min is
determined based on whether a patient has had nausea, vomiting
or dizziness. During this period, fluid infusion and oxygen will lead
to a full recovery of patient strength and will avoid the possibility
of postoperative orthostatic hypotension caused by preoperative
fasting. In view of probable retrograde amnesia after anesthesia,
it is necessary to register and check valuables carried by patients
before the operation to avoid unnecessary issues later.
Anesthesia affected patient orientation and motor coordination
and was probably responsible for a sense of fatigue and increased
excitement thus leading to a decrease in patient safety consciousness
or awareness. Therefore, it is suggested that patients be forbidden
to drive or work high above ground for 24h after the operation.
At the same time, patients must be accompanied by others when
leaving the hospital. To sum up, it is not appropriate that all patients
should be routinely observed for 30 min after painless induced
abortion using propofol and sufentanil. The observation period
should depend on the varying reactions of patients to the operation
and the anesthesia and on whether or not they are accompanied by
others to ensure their medical and personnel safety.
References
- Fan GS, Jin L, Xi S, Hong Li (2005) Clinical observation of propofol combined with misoprostol for painless induced abortion. Zhonghua Yi Xue Za Zhi 85(16): 1106-1108.
- Wang L, Li W, Xu R, Lihui Long (2016) [Meta analysis for the anesthesia effect and adverse reactions of etomidate and propofol on the painless abortion surgery]. Zhong Nan Da Xue Xue Bao Yi Xue Ban 41(4): 427-433.
- Loser S, Herminghaus A, Huppe T, W Wilhelm (2014) [General anesthesia for ambulatory surgery: Clinical pharmacological considerations on the practical approach]. Anaesthesist 63(11): 865-870, 872-864.
- Xie K, Zhang W, Fang W, Yanhong Lian, Sufeng Lin, et al. (2017) The analgesic efficacy of oxycodone hydrochloride versus fentanyl during outpatient artificial abortion operation: A randomized trial. Medicine (Baltimore) 96(26): e7376.
- Schulte PJ, Roberts RO, Knopman DS, R. C. Petersen, A. C. Hanson, et al. (2018) Association between exposure to anaesthesia and surgery and long-term cognitive trajectories in older adults: report from the Mayo Clinic Study of Aging. Br J Anaesth 121(2): 398-405.
- Yang Z, Yi B (2016) Patient experience of sexual hallucinations after propofol-induced painless abortion may lead to violence against medical personnel. J Anesth 30(3): 486-488.
- Vutskits L, Xie Z (2016) Lasting impact of general anaesthesia on the brain: mechanisms and relevance. Nat Rev Neurosci 17(11): 705-717.
- Wang C, Wu X (2002) Influence of General Anesthesia on the Cognitive Function of the Middle-aged. Chinese Journal of Anesthesiology 22(6): 332-335.
- Simon Bn T (2003) General Anaesthesia and Cognitive Functioning. Chinese Journal of Clinical Psychology 11(1): 71-72.
- Evered LA, Silbert BS (2018) Postoperative Cognitive Dysfunction and Noncardiac Surgery. Anesth Analg 127(2): 496-505.
- Finco G PE, Rigo V (1997) New opioids in 1-day surgery. Ambul Surg 4: 125-129.
- Bouillon T, Bruhn J, Radu-Radulescu L, Edward Bertaccini, Sang Park, et al. (2002) Non-steady state analysis of the pharmacokinetic interaction between propofol and remifentanil. Anesthesiology 97(6): 1350-1362.
- Sear JW (1998) Recent advances and developments in the clinical use of i.v. opioids during the peroperative period. Br J Anaesth 81(1): 38-50.
- Lei M, Zhang P, Liu Y, Fangfang Fu, Ling Ye, et al. (2017) Propofol and sufentanil may affect the patients' sleep quality independently of the surgical stress response: a prospective nonrandomized controlled trial in 1033 patients' undergone diagnostic upper gastrointestinal endoscopy. BMC Anesthesiol 17(1): 53.
- Yin S, Hong J, Sha T, Zhicong Chen, Yihua Guo, et al. (2019) Efficacy and Tolerability of Sufentanil, Dexmedetomidine, or Ketamine Added to Propofol-based Sedation for Gastrointestinal Endoscopy in Elderly Patients: A Prospective, Randomized, Controlled Trial. Clin Ther 41(9): 1864-1877 e1860.

 Short Communication
Short Communication