Abstract
Studies have related blood group and some infectious diseases. The relationships between malaria infection and blood group have been studied over time, but they are in contrast with each other. Therefore, the need to carry-out the research in Makurdi as malaria has being one of the major causes of child mortality among pupils. Rapid One Step Malaria Ag. HRP2 Card Test was used to test for malaria while Smar kit was used to determine different blood groups. A total of 150 school children were sampled in North Bank area of Makurdi between June and July 2014. Out of 152 school children used in the study, 127 were positive to malaria infection, the blood group distribution was in the ratio of 32, 38, 7 and 73 for blood groups A, B, AB and O respectively. Blood groups A and B had the highest prevalence of malaria while the least were in O and AB. Only 70 (46.7%) of the students had LLINS and only 30 % of the owners do sleep under LLINS.
Keywords: Environment; Antibodies; Carbohydrate; Infectious Disease; Blood Sample; Plasmodium; Antigens; P. falciparium
Introduction
Several researches have shown the relationship between ABO blood group and infectious diseases [1]. Malaria has been one of the deadliest diseases in the tropics and sub tropics [2]. Malaria control has been a difficult task in the tropics mainly due to the environmental conditions that favour the Mosquito vector. The ABO blood groups consist of A, B and H carbohydrate antigens which can regulate protein activities during infection and antibodies against these antigens [3]. A number of studies have reported contradictory reports on significant association between ABO blood group system and some disease conditions, the studies reviewed the impact of ABO blood group on infection status of individuals [4]. However, other studies have shown that high frequency of malaria has been observed among blood group ‘A’ individuals as compared with oth er blood group individuals. Large numbers of severe malaria cases were also reported among blood group ‘A’ individuals [5].
Material and Method
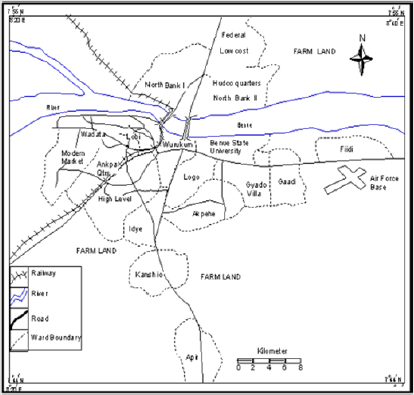
The research was carried out in North Bank Area of Makurdi
Benue Nigeria (Figure 1). Blood sample was collected using lancet
as described in the RDT AG HRP2 CARD TEST manual as follows:
The thump was cleaned with an alcohol swab. The end of the
fingertip was squeezed and pierced with sterile lancet. The first
drop of blood was wiped away with cotton. The pierced fingertip
was squeezed gently, and sample pipette was used to collect 10μlof
blood. The test device was placed on a flat surface and labeled with
student’s identification number and 5μl blood was added into the sample well of the respective Test Device. Two drops (60μl) of Assay
Diluent was added to Assay Diluent well. The result was read within
20 minutes. The remaining portion of blood was dropped in four
different glass slides labeled A, B, AB and D and respective Antigens
were added as described in the manufacturer’s manual for ABO
blood grouping. The result was read in 5minutes and interpreted
[6].
Results
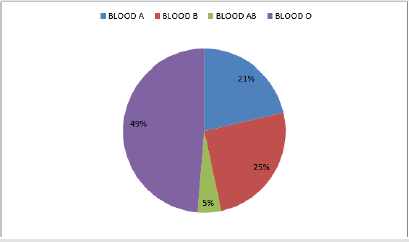
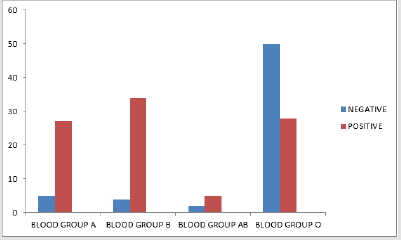
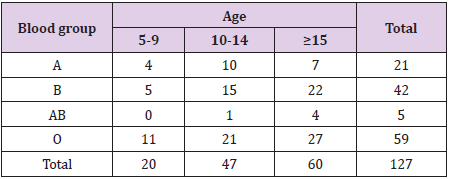
In the study to ascertain the relationship between ABO blood group and Plasmodium falciparium infection using Smart diagnosis Blood grouping reagent Test and Smart Rapid Diagnosis Test Kits among school children in North bank area of Makurdi, Benue State, Blood groups A,B, AB, and O were present in the study population in the ratio 0f 4.5:5.4:1:10.4 respectively. Out of 152 school children sampled, 127 were positive to malaria infection while only 2 students were negative to the test and 2 results showed invalid. Children with blood group A, B, AB and O were 32, 38, 7 and 73 respectively. Figure 2 shows percentage distribution of blood group among the students while Figure 3 shows malaria infection. The prevalence was as follows for P.falciparium infection 21.1%, 25%, 4% and 48% for blood groups A, B, AB and O respectively (Table 1). There were no significant different in relation to blood group malaria infection (P>0.05). with respect to Long Lasting Insecticide-treated Nets (LLINs) ownership and usage, 46.7% of the students had LLINS and only 30 % of the owners do sleep under LLINS (Table 2).
Discussion
The result of our study is an indication that individual susceptibility to malaria parasite mainly P.falciparium varies according to blood group, the cause of the variance is yet to be ascertained though there are some suggestions firstly variations in genetic makeup of the individual and variations in chemical structure of the receptor sites of the erythocytic of the various blood groups of an individual may cause the variation in susceptibility to Plasmodium infection. This study revealed that blood group O had 48% of the total population which indicates its high abundance in areas where malaria infection in endemic, this is in support of previous work by Christine and Walter in 2007 [7] which states that ‘the ratio of group O to A is higher in geographic regions where malaria is currently endemic’. Also, the role of group A and B antigens in cytoadherence rosette formation with P. falciparum erythrocytes membrane protein (PfEMP-1) than in blood group O may explain why group A and B individual are prone to malaria infection [3] this could suggest a higher rate of survival from malaria among individuals associated with blood group A and B which agrees with Uneke, et al. [8].
In terms of prevalence of malaria infection with respect to
blood groups, groups A and B had 50% infection in school children
below 10 years of age while group O of the same age range had
40% infections, this agrees with earlier report by Williams in
2006 [9] and also that of Christine and Walter in 2007 [7], which
revealed that many polymorphic human genes are implicated when
it comes to the in the determination of infectivity or resistance to
Plasmodium infection to some extent which may include blood
group A and O respectively, this also agrees with previous study
in Taraba Nigeria [10] which stated that Blood group A was more
significantly infected than other blood groups, followed by blood
group B and least infected was blood group O . Blood group AB had
a low prevalence infection as in blood group O. the results suggests
a slight resistance to malaria infection in blood groups AB and O.
This is in contrast to report by Williams in 2006 [9] which gave
higher rate of infection in blood group O. This is an indication that
blood group A is a risk factor for severe malaria while blood group
O may provide some form of protection against malaria; this is in
agreement with work done by Senga et al. in 2007 [10]. The overall
prevalence was as follows 34% for blood groups A and B while AB
and O had 28.6 5 and 28.8% respectively.
However, correlation is significant at 0.01 between ABO blood
group and P. falciparium infection. This suggests a strong positive
relationship between blood group and malaria infection, which is
in contrast with work of Burhan, et al. [11] which suggested no
association between blood group and malaria infection. The agerelated
infection showed that age group 10-14 had the highest
prevalence of malaria infection; this could be implicated with the
number of hours the age group stays out thereby exposing the
group to mosquito bite. This is because this group is very active
house-hold chores which most often make them stay out late. Next
to this age group in prevalence is 15years and above, this could also
be likened to the above reasons.
Ownership /Usage of Long Lasting Insecticide-treated Nets
With respect to ownership of Long Lasting Insecticide-treated Nets (LLINs), only 70 (46.7%) of the students had LLINs as that time of this study, while a larger population (53.3%) of the study had no LLINs. This was despite the free distribution of LLINs ongoing in the area as at that period. Surprisingly, only 21 (30%) out of the owners of LLINs actually sleep in it. Further [robbing identified some discomforts such as heat, the odor of the fabrics as reasons for non-usage. Some also believed that LLINs are used to preserve corpses therefore, they cannot sleep in it.
Conclusion
The result of this study showed a higher rate of malaria infection in school children with ABO Blood group ‘A’ and ‘B’. It was also discovered that most of the students do not sleep under insecticide treated nets.
Acknowledgement
We sincerely wish to acknowledge the school authorities and students especially Benlad Model Secondary School North Bank Makurdi Benue State Nigeria and others for their support during the study.
References
- Deepa, Alwar VA, Karuna Rameshkumar, Ross C (2011) ABO blood groups and malaria related clinical outcome. Journal of vector Borne Dis 48(1): 7-11.
- Guptaa M, Rai Chowdhuru AN (1980) Relationship between ABO Blood group and Malaria. Bulletin of the World Health Organization 58(6): 913-915.
- Degarege A, Medhin G, Animut A, Legess M, Erko B (2012) Association of ABO blood group and P. falciparum malaria related outcomes: across-sectional study in Ethiopia. Acta Trop 123(3): 164-169.
- Gayathri BN, Harendra Kumar ML, Gomathi N, Jeevan Shetty, Reethesh RP (2013) Relationship between ABO blood groups and malaria with clinical outcome in rural area of South India. Global Journal of Medicine and Public Health 2(1): 1-7.
- (2012) World Health Organization (WHO). World Malaria Report.
- Wood CS, Harrison GA, Dore C, Weiner JS (1972) Selective feeding of Anopheles gambiae according to ABO blood group status. Nature 239(5368): 165.
- Christine MC, Walter HD (2007) The ABO blood system and Plasmodium falciparum. J Amer Soc Haematol 110(7): 2250-2258.
- Uneke CJ, Ogbu O, Nwojiji V (2006) Potential risk of induced malaria by blood transfusion in Southeastern Nigeria. Mc Gill J Med 9(1): 8-13.
- Williams TN (2006) Human red blood cell polymorphisms and malaria. Current Opin Microbiol 9(4): 388-396.
- TIDI SK, Amos JT, Firyanda E (2013) Association between Plasmodium infection, Haemoglobin genotypes and Blood groups among Under-five nomadic Fulani of Northeastern Nigeria. International journal of malaria research and reviews 1(2): 7-11.
- Burhan H, Hasan AS, Mansur UI Hague S, Zaidi G, Shaikh I, et al. (2016) Association between Blood Group and Susceptibility to Malaria and its Effects on Platelets, TLC and HB. Journal of infectious Diseases of Developing Countries 10(10): 1124-1128.

 Research Article
Research Article